
Analysis of risk factors for early urinary tract infection after kidney transplantation
Introduction
Kidney transplantation is currently the best available therapy to prolong the life of patients with end-stage renal disease (1). The primary postoperative goal is to maintain good graft function on the basis of effective prevention of infection (2). The early stage after kidney transplantation, that is, the first month after operation, is the peak stage for infectious complications (3), 45–72% of which are urinary tract infections (UTIs) (2), which have an incidence rate of 6–86% (4). UTIs can prolong the recipient’s hospital stay, increase medical expenses, and, in severe cases, lead to graft failure or even threaten the recipient’s life (5).
There are many studies on the risk factors of UTI following kidney transplantation, but few of them have focused on the risk factors of early UTI after the operation. Better understanding early UTIs after kidney transplantation will help medical staff adopt more scientific and effective UTI prevention and control measured. This study describes the current status of early UTI after kidney transplantation and investigates its risk factors, aiming to provide a theoretical basis for reducing the occurrence of early postoperative UTI. We present the following article in accordance with the STROBE reporting checklist (available at http://dx.doi.org/10.21037/tau-20-1248).
Methods
Subjects
We retrospectively analyzed patients undergoing kidney transplantation between January 2018 and December 2019 in a first-class tertiary hospital in Suzhou, China, by convenience sampling. Inclusion criteria: patients were ≥18 years old and were within one month after kidney transplantation. Exclusion criteria: patients with incomplete data, patients with confirmed UTI before transplantation, and patients undergoing multiorgan transplantation. This study was approved by the medical ethics committee of the First Affiliated Hospital of Soochow University, and the approval number was No. 2020-187. All procedures performed in this study involving human participants were in accordance with the Declaration of Helsinki (as revised in 2013). Individual consent for this retrospective analysis was waived.
Study methods
Inclusion of influencing factors
Based on a review of the previous literature (6-8) and the status of our transplantation center, our research group decided that 20 factors might be associated with early UTI after kidney transplantation: sex, age, body mass index (BMI), history of diabetes, history of hypertension, history of hepatitis B, duration between primary disease and transplantation, average preoperative daily urine volume, preoperative dialysis, immune induction plan, immune suppression plan, duration of surgery, cold ischemia time, warm ischemia time, postoperative ureteral stent (double-J stent, D-J stent) placement time, postoperative urethral catheter placement time, postoperative acute rejection reaction, delayed graft function (DGF), duration of postoperative preventive antibacterial medication use, and duration of postoperative hospital stay. We designed the “Early UTI registration form for recipients after kidney transplantation” using the above factors as independent variables and whether UTI occurred as the dependent variable and collected the data of kidney transplant recipients.
UTI monitoring and diagnostic criteria
The urine of the recipient after kidney transplantation was collected for monitoring once per day for the first two weeks and then once every Monday, Wednesday, and Friday until discharge. Standard procedures were strictly followed when collecting urine samples (2). The detailed UTI diagnostic criteria were as follows: the patient had symptoms of the urinary tract, including frequent urination, urinary urgency, and dysuria, or tenderness in the lower abdomen or percussive pain in the kidney region, with or without fever, and had one of the following: (I) urine white blood cell count ≥10/high-power field in females or ≥5/high-power field in males; (II) gram-positive cocci ≥104 colony-forming units (CFU)/mL and gram-negative bacilli ≥105 CFU/mL from the culture of the clean middle part of the urine or urine collected from the urethral catheter; (III) gram-positive cocci ≥104 CFU/mL and gram-negative bacilli ≥105 CFU/mL from urine culture of asymptomatic bacteriuria patients with a recent (1-week) history of endoscopy or indwelling urethral catheterization; (IV) the patient was clinically diagnosed with UTI or was confirmed with UTI due to effective anti-bacterial treatment (2).
Data collection
Two researchers who underwent the same training independently screened the medical records according to the inclusion and exclusion criteria and collected and recorded relevant data. Differences between the two researchers were discussed and resolved together or by consulting a third party.
Statistical analysis
Data were analyzed with SPSS 21.0 software. Categorical data are expressed as frequency and percentage, and differences between groups were determined by the chi-squared test or Fisher’s exact test. Quantitative data are expressed as mean ± standard deviation or median with interquartile range, and differences between groups were determined by the t-test or the nonparametric rank sum test. Risk factors for early UTI after kidney transplantation were analyzed by a logistic regression model. Differences with P<0.05 were considered statistically significant.
Results
General data of the subjects
This study included 129 recipients, including 85 males (65.9%) and 44 females (34.1%) with an age range of 18–64 years (41.88±10.75). Their primary diseases included 20 cases of glomerulonephritis, 11 cases of diabetic nephropathy, five cases of hypertensive nephropathy, 20 cases of IgA nephropathy, five cases of polycystic kidney, and 68 unknown diseases. All recipients were transplanted for the first time, and the source of the kidney was Donation after Citizen's Death (DCD). Preoperative panel-reactive antibody (PRA) was negative. A urethral catheter and D-J stent were placed during surgery. In the perioperative stage, methylprednisolone + anti-thymic lymphocyte immunoglobulin/Simulect/thymoglobulin immune induction regimen was used. A triple immunosuppressive regimen of mycophenolate mofetil + tacrolimus/cyclosporin A + prednisone was used after operation. Second- and third-generation cephalosporin were used for postoperative infection prevention.
Occurrence of early UTI after kidney transplantation
Among the 129 recipients, 62 patients had UTI within one month after kidney transplantation (48.1%), of whom 25 were male (40.3%) and 37 were female (59.7%). The median time of UTI occurrence was 5 [4–10] days after operation, the shortest being 1 day and the longest being 22 days. Among the 2,915 urine culture samples, 243 specimens had pathogens, and 186 specimens were contaminated. A total of 324 strains of UTI pathogens were detected, including 279 gram-negative bacilli (86.1%), 34 gram-positive cocci (10.5%), and 11 fungi (3.4%). The pathogen with the highest detection rate was Escherichia coli, with a total of 206 strains (63.6%). Two patients lost graft function.
Univariate analysis of early UTI after kidney transplantation
Univariate analysis showed that female sex, older age, longer duration between primary disease and transplantation, lower total amount of methylprednisolone, later postoperative D-J stent placement time, DGF, shorter postoperative preventive antibacterial medication use, and longer postoperative hospital stay were significantly associated with early UTI after transplantation (P≤0.05, Table 1).
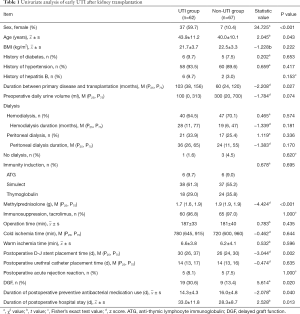
Full table
Multivariate analysis of early UTI after kidney transplantation
To avoid excluding factors that were not statistically significant in univariate analysis but that could be significant in multivariate analysis, we included all the factors with P≤0.1 in univariate analysis in the logistic regression model (9). These totaled nine independent variables. The regression results showed that female sex and DGF were statistically significant risk factors, with χ2=54.285, P<0.001 (Table 2). This model could accurately predict 81.4% of recipients who would have early UTI after kidney transplantation, with a sensitivity of 86.6%, a specificity of 75.8%, a positive predictive value of 83.9%, and a negative predictive value of 79.5%.
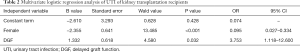

Full table
Discussion
Incidence and occurrence time of early UTI after kidney transplantation
The recipient and graft survival rates are higher than 90% at 1 year after kidney transplantation (10). However, the survival of both recipient and graft still face many risks, among which UTI is the most common postoperative infectious complication (11). UTI can cause bacteremia and even sepsis, which seriously impact the prognosis of the recipient and the graft function (11,12). The incidence of early UTI after kidney transplantation in our study was 48.1%, which is similar to the incidence in a previous study (4). Differences in the incidence may be related to the level of medical care in each center or to the differences in research methods such as the frequency of urine testing and the UTI diagnostic criteria. Although the incidence of early UTI after kidney transplantation has decreased in recent years, it is still high (13). The reason for the high early UTI incidence may be that the medical staff still need to improve in the early prevention and treatment of UTIs after kidney transplantation, such as in their theoretical knowledge, patient monitoring, and patient education. Our study showed that the median time of early-stage UTI was 5 [4, 10] days after surgery. This finding indicates that 4–10 days after kidney transplantation is a critical period for preventing UTI. In a study of the early UTI occurrence time after kidney transplantation, Bodro et al. included 867 recipients early after kidney transplantation for a retrospective cohort study (13) and showed that UTI occurred an average of 18 days after transplantation, which is later than we found. The reason for this discrepancy may be that in our study, all the donor kidneys were from DCD, whereas in the study by Bodro et al., 205 donors (23.64%) were living (13). Living-donor kidney transplantation has good histocompatibility and requires a low postoperative immunosuppressant dosage. As a result, UTI may have occurred later than they do after DCD kidney transplantation (13).
Female recipients are at higher risk for early UTI after kidney transplantation
The incidence of UTI among kidney transplantation recipients is higher than that of the general population, and more than 50% of women, especially postmenopausal women, have at least one UTI in their lives (14). Our study showed that the incidence of early UTI after kidney transplantation among female recipients was higher than that among male recipients, which is consistent with the study by Fiorant et al. (15). The logistic regression analysis in our study showed that female sex was a risk factor for early UTI after kidney transplantation. In a retrospective cohort study with 99 recipients, Menegueti et al. (11) found that the only risk factor associated with UTI after kidney transplantation was female sex. Another study showed that the incidence of UTI among postmenopausal female recipients was higher than among nonmenopausal women (16). The reasons for these findings may be following: (I) the female urethra is short and close to the anus, so it is easily affected by the intestinal flora, such as E. coli, leading to retrograde infection (12). The pathogen with the highest frequency in our study was E. coli, accounting for 63.6%, which is similar to the results of related studies (17). (II) The differences between male and female urine proteomic patterns, as found recently, may also affect urinary bacterial proliferation and inflammatory processes (18). (III) Estrogen can promote the differentiation and keratinization of vaginal epithelial cells, increase glycogen and its decomposition in epithelial cells, and keep the environment of the vagina acidic. Reduced estrogen after menopause changes the acidic environment of the vagina. The dominant flora changes from lactic acid bacteria to E. coli. As a result, the original infection-protection mechanism is weakened (15). The following prevention and control measures can be taken based on the above possible reasons: The recipient can be instructed to flush the perineum with benzalkonium bromide, and any infections should be treated quickly. After the operation, the urethral orifice should be cleaned every day with benzalkonium bromide, and the perineum should be rinsed after each bowel movement. Additionally, physiological bladder irrigation (drinking water) is highly helpful in the prevention of UTI. Therefore, recipients who can drink water normally should be encouraged to drink more than 2,000 mL of water each day and maintain a urine output of more than 2,000 mL. Continuing nursing services after discharge can also improve the knowledge of kidney transplant recipients about UTI prevention (19).
DGF is a risk factor for early UTI after kidney transplantation
A previous study indicated that DGF increased the risk of early UTI after kidney transplantation (20), which is also confirmed by our study. We showed here that the incidence of UTI among the 28 patients with DGF was 67.9%. The detailed mechanism by which DGF impacts the occurrence of UTI is not clear. Some studies suggest that recipients with DGF require longer to recover their graft function, and their longer hospital stay increases the chance that the recipient will come into contact with pathogenic bacteria in the hospital. When recipients with DGF come in contact with pathogenic bacteria, the bacteria attach to the urothelium through adhesion factors. Due to the low urine output and poor immune function of the recipient, pathogenic bacteria can easily enter and stimulate the bladder through the urethra, which causes cystitis. If the pathogenic bacteria continue to move up the ureter, they may cause acute pyelonephritis (21). Some scholars (20) also believe that recipients with DGF usually have prolonged immune induction times with polyclonal antibodies as well as a greater amount of antibodies, and polyclonal antibodies are an important cause of infections among kidney transplant recipients. Therefore, if DGF recipients have fever, multiple urine cultures should be performed to eliminate the possibility of UTI, in addition to lung computed tomography and sputum culture examinations.
Limitations
This study only selected 129 recipients from one first-class tertiary hospital after kidney transplantation. These patients were similar in some ways. For example, the recipients all underwent their first transplantation, all were PRA-negative, and all the donor kidneys were from DCD, which may have caused some biases in our findings. Therefore, multicenter and larger studies are required to confirm our findings. Second, this was a retrospective study. Some UTI data, such as the etiological results of the donors, the urinary tract obstruction status of the recipients, and whether the female recipients were menopausal, may have been incomplete. Therefore, the influencing factors included in this study are limited in usefulness, and the impact of some other factors on early UTI might have been neglected. Prospective studies are needed for more detailed insight.
In summary, our study did not find any deaths related to early UTI after kidney transplantation. The incidence of early UTI after kidney transplantation is still high. Four to 10 days after the operation is the critical period for preventing UTI. Females and patients with DGF are high-risk groups for early UTI after kidney transplantation. Medical care for these groups should be strengthened in the early stage after transplantation in order to reduce the occurrence of UTI and to improve the survival rate and graft quality of the recipients.
Acknowledgments
The authors gratefully thank Yu-Hua Huang (the department of urology, First Affiliated Hospital of Soochow University, Suzhou, China) for his kind help in quality control and data collection.
Funding: None.
Footnote
Reporting Checklist: The authors have completed the STROBE reporting checklist. Available at http://dx.doi.org/10.21037/tau-20-1248
Data Sharing Statement: Available at http://dx.doi.org/10.21037/tau-20-1248
Conflicts of Interest: All authors have completed the ICMJE uniform disclosure form (available at http://dx.doi.org/10.21037/tau-20-1248). The authors have no conflicts of interest to declare.
Ethical Statement: The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. This study was approved by the medical ethics committee of the First Affiliated Hospital of Soochow University (approval No. 2020-187). All procedures performed in this study involving human participants were in accordance with the Declaration of Helsinki (as revised in 2013). Individual consent for this retrospective analysis was waived.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- Del Bello A, Kamar N. Do natural antibodies have a detrimental effect after kidney transplantation? Ann Transl Med 2018;6:316. [Crossref] [PubMed]
- Mukherjee D, Sharma S, Nair RK, et al. Urinary tract infection in renal transplant recipients at a tertiary care center in India. Saudi J Kidney Dis Transpl 2018;29:361-8. [Crossref] [PubMed]
- Khosroshahi HT, Mogaddam AN, Shoja MM. Efficacy of high-dose trimethoprim-sulfamethoxazol prophylaxis on early urinary tract infection after renal transplantation. Transplant Proc 2006;38:2062-4. [Crossref] [PubMed]
- Bahrami A, Shams SF, Eidgahi ES, et al. Epidemiology of Infectious Complications in Renal Allograft Recipients in the First Year After Transplant. Exp Clin Transplant 2017;15:631-5. [PubMed]
- Britt NS, Hagopian JC, Brennan DC, et al. Effects of recurrent urinary tract infections on graft and patient outcomes after kidney transplantation. Nephrol Dial Transplant 2017;32:1758-66. [Crossref] [PubMed]
- Thompson ER, Hosgood SA, Nicholson ML, et al. Early versus late ureteric stent removal after kidney transplantation. Cochrane Database Syst Rev 2018;1:CD011455. [Crossref] [PubMed]
- Kırnap M, Boyvat F, Torgay A, et al. Incidence of Urinary Complications With Double J Stents in Kidney Transplantation. Exp Clin Transplant 2019;17:148-52. [Crossref] [PubMed]
- Ooms L, IJzermans J, Voor In 't Holt A, et al. Urinary Tract Infections After Kidney Transplantation: A Risk Factor Analysis of 417 Patients. Ann Transplant 2017;22:402-8. [Crossref] [PubMed]
- Pinckaers FME, Boon ME, Majoie MHJM. Risk factors predisposing to psychotic symptoms during levetiracetam therapy: A retrospective study. Epilepsy Behav 2019;100:106344. [Crossref] [PubMed]
- Chen YX, Li R, Gu L, et al. Risk factors and etiology of repeat infection in kidney transplant recipients. Medicine (Baltimore) 2019;98:e17312. [Crossref] [PubMed]
- Menegueti MG, Pereira MF, Bellissimo-Rodrigues F, et al. Study of the risk factors related to acquisition of urinary tract infections in patients submitted to renal transplant. Rev Soc Bras Med Trop 2015;48:285-90. [Crossref] [PubMed]
- Dharnidharka VR, Agodoa LY, Abbott KC. Effects of urinary tract infection on outcomes after renal transplantation in children. Clin J Am Soc Nephrol 2007;2:100-6. [Crossref] [PubMed]
- Bodro M, Sanclemente G, Lipperheide I, et al. Impact of urinary tract infections on short-term kidney graft outcome. Clin Microbiol Infect 2015;21:1104.e1-8. [Crossref] [PubMed]
- Chan S, Pascoe EM, Clayton PA, et al. Infection-Related Mortality in Recipients of a Kidney Transplant in Australia and New Zealand. Clin J Am Soc Nephrol 2019;14:1484-92. [Crossref] [PubMed]
- Fiorante S, López-Medrano F, Lizasoain M, et al. Systematic screening and treatment of asymptomatic bacteriuria in renal transplant recipients. Kidney Int 2010;78:774-81. [Crossref] [PubMed]
- Perrotta C, Aznar M, Mejia R, et al. Oestrogen for preventing recurrent urinary tract infection in postmenopausal women. Obstet Gynecol 2008;112:689-90. [Crossref] [PubMed]
- Shams SF, Eidgahi ES, Lotfi Z, et al. Urinary tract infections in kidney transplant recipients 1st year after transplantation. J Res Med Sci 2017;22:20. [Crossref] [PubMed]
- Thölking G, Schuette-Nuetgen K, Vogl T, et al. Male kidney allograft recipients at risk for urinary tract infection? PLoS One 2017;12:e0188262. [Crossref] [PubMed]
- Li L, Ma Z, Wang W. Influence of transitional care on the self-care ability of kidney transplant recipients after discharge. Ann Palliat Med 2020;9:1958-64. [Crossref] [PubMed]
- van den Hoogen MW, Hoitsma AJ, Hilbrands LB. Anti-T-cell antibodies for the treatment of acute rejection after renal transplantation. Expert Opin Biol Ther 2012;12:1031-42. [Crossref] [PubMed]
- Bien J, Sokolova O, Bozko P. Role of Uropathogenic Escherichia coli Virulence Factors in Development of Urinary Tract Infection and Kidney Damage. Int J Nephrol 2012;2012:681473. [Crossref] [PubMed]


