Transrectal ultrasound-guided extraction of impacted prostatic urethral calculi: a simple alternative to endoscopy
Introduction
Obstructive uropathy is a common clinical problem, and urethral calculi constitute the least common form of calculus disease leading to obstructive uropathy. The adult urethra has a relatively uniform diameter of approximately 30 French and may, therefore, allow passage of stones <10 mm. Because the urethra contains the largest luminal diameter of the urinary tract, it is rare for a stone to impact and obstruct the passage of urine. As a result, urethral calculi comprise 1–2% of all genitourinary calculi (1). More common in males (2), urethral calculi are typically found in the posterior urethra (1,2) because the membranous urethra is the narrowest and least dilatable part of the urethra. Also, physiologic urethral stenosis occurs at the junction of the fossa navicularis and external urethral meatus, and at the internal urethral sphincter. Therefore, urethral calculi commonly impact proximal to the area of stenosis (3). Although urethral stones are more common in the posterior urethra, approximately 12% of urethral stones become trapped in the anterior urethra. Stones impacted in the anterior urethra are generally smaller than those caught in the posterior urethra (4). Presently, urethral calculi are managed with invasive endourologic methods or external urethrotomy, which require general anesthesia and inpatient treatment. We report a novel technique to remove prostatic urethral calculi by visualization using real-time transrectal ultrasonography (TRUS).
Rationale and utilization of novel procedure
A 64-year-old male underwent ureteroscopy and laser lithotripsy for an 8 mm symptomatic renal stone. Postoperatively, he developed pain at the tip of the penis associated with urinary dribbling. A posterior urethral stone was suspected as the cause of his presentation; TRUS revealed a 5 mm calculus at the level of the prostatic urethra (Figure 1A).
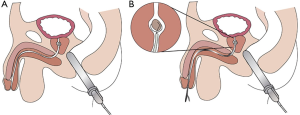
Currently, urethral calculi are managed with invasive endourologic methods or external urethrotomy. Rather than having the patient go through open surgery, postoperative analgesia, radiation exposure, or hospitalization, we applied 2% xylocaine jelly into the entire length of the urethra. The distal opening of a 20 French latex Council-tip 2-way Foley catheter was dilated, lubricated, and gently inserted into the urethra following adequate local anesthesia. TRUS was used to position the catheter close to the impacted stone, which was located in the intersphincteric prostatic urethra. Pre-procedure dilation of the Foley catheter allowed a Captura® three-prong grasper (2.8F, Cook Medical, Bloomington, IN) to be threaded through the urine drainage port. Using TRUS, the impression of the grasper's distal tip was positioned below the stone, enabling us to monitor the contact of the grasper's prongs with the stone in real-time. The stone was manipulated and trapped into the basket while creating minimal contact with the urethra (Figure 1B). The trapped stone was withdrawn into the lumen of the Foley catheter, and the system was removed without damage to the urethral mucous membrane. At the conclusion of the procedure, TRUS was used to image the bladder and exclude the presence of additional stones that may obturate the urethra.
The operative time was 45 minutes, the blood loss was <5 mL, and the patient was sent home immediately. There were neither complications associated with the procedure nor symptom recurrence at the two-week follow-up.
Discussion and future perspectives
The use of TRUS in the diagnosis and extraction of prostatic urethral stones has not been previously described in the literature, although a few examples of sonographic diagnosis of calculi are documented. One case report describes the use of dynamic high-frequency ultrasound to localize and remove distal urethral stones, but similar techniques to eliminate calculi from the posterior urethra have not been reported (5). Voiding sonourethrography has also been used to diagnose prostatic urethral calculi by visualizing the movement of calcified structures upon urination (6).
In Table 1, we summarize the current widespread use of TRUS in urological practice. Though retrograde urethrography and voiding cystourethrography are the gold standard imaging techniques for anatomic and functional studies of the urethra, these procedures are invasive, involve radiation exposure, and cannot be performed in the convenience of an office setting. Also, varying degrees of radiolucency have been reported amongst urethral calculi with rates of radiopacity ranging from 40% (7) to 98% (4). TRUS offers a simpler, radiation-free imaging method unlike retrograde urethrography and voiding cystourethrography. Although current literature lacks documentation for the sensitivity of ultrasonography in detecting urethral calculi, this imaging modality has been shown to achieve sensitivity rates of 98.3% in detecting upper urinary tract stones (8). However, it is important to sonographically distinguish prostatic urethral calculi from intraprostatic calcifications, which are commonly found periurethrally or underneath the prostatic pseudocapsule. Although TRUS can correctly differentiate and identify a prostatic urethral calculus, imaging of intersphincteric stones in patients with extensive prostatic calcification becomes challenging. Fortunately, as most patients present with punctate calcification, if any, our method of extraction is very much feasible.

Full table
Once a diagnosis has been made, selecting the appropriate treatment is based on the size, shape, location, and position of the stone. Also, the presence or absence of associated urethral anatomical pathology and experience of the operator are relevant considerations. Current interventions include milking, endoscopic forceps extraction, endoscopic push-back with cystolithotripsy, endoscopic push-back with open or percutaneous transvesical extraction, extracorporeal shock wave lithotripsy (ESWL), in situ lithotripsy, internal or external urethrotomy, and meatotomy. Studies document that endoscopic push-back is the most common procedure and has an 86% success rate (4). Possible complications with endoscopic cystolithotripsy include erosion or perforation of the bladder wall along with urethral stress and late stricture formation (9). Alternatively, TRUS-guided urethral stone extraction bears no such complications.
Extracorporeal shock-wave lithotripsy (ESWL) monotherapy has been used to treat urethral and bladder stones presenting with acute urinary retention after Foley catheter push-back (10). This minimally-invasive procedure does not require anesthesia and can be performed on an outpatient basis—advantages shared with TRUS-guided stone extraction. However, the creation of numerous fragments can complicate urinary retention. ESWL reportedly has a 48% success rate in pediatric patients and may require several sessions for complete stone eradication (11). In contrast, the need to reoperate is avoided in procedures that extract the stone in its entirety.
Qualities of a stone, such as spikes or an irregular shape, can prevent its natural passage in the urethra, which is also evident for stones sizes less than the diameter of an adult urethra, as represented in our report. Nevertheless, causes that lead a stone to be impacted in the prostatic urethra have not been studied extensively. In this report, we capture a 5 mm calculus within the distal latex of a 20 French council tip catheter. Stones that match or slightly exceed the diameter of the Foley catheter (20 French is equivalent to 6.6 mm diameter) can be safely enveloped. Since the adult urethra has a uniform diameter of approximately 30 French (9.9 mm diameter), any catheter that would safely encapsulate a prostatic stone may be theoretically retrieved. A calculus less than 10 mm in size can be safely removed with a Foley catheter without hindrance in a patient with no history of a urethral disease or abnormal anatomy. In the strategy we have presented, a three-prong grasper is used to envelop the body of the stone within the lumen of a Foley catheter. This provides a latex barrier between the stone and the urethra to ultimately prevent mucosal damage or future complications such as urethral stricture from an otherwise abrasive, spiked, or irregularly shaped calculus, which characterizes most stones impacted along the prostatic urethra, during removal of the Foley-stone system. Current endoscopic treatments do not offer this possible protection. However, studies are needed to assess if this feature reduces the rate of these common complications. We do not recommend this technique in cases of impacted or large stones, or in patients with significant urethral pathology. Anatomic constraints or significant edema of the urethral mucosa may preclude manipulation with the three-prong grasper. Calculi that fail to dislodge can be treated effectively with in situ lithotripsy using a holmium laser to minimize collateral urethral tissue damage (12). Open surgery may be required when emergent stone clearance is necessary or in situations when a stone size exceeds 4 cm in diameter. Although these surgeries are met with disadvantages such as scar formation, long postoperative hospital stays, urethral catheterization, and extensive analgesic requirements (9), the large size precludes the possibility of successful push-back or manipulation into a Foley catheter of a smaller diameter.
Should the procedure fail and the stone becomes impacted in a more distal area of the urethra during Foley catheter removal, the calculus should be released from the grasper to limit mucosal injury. Appropriate management will then depend on the algorithm outlined above, which considers the stone’s size, quality, and location, with endoscopic intervention as the first line. Because the stone is likely too large or abrasive, milking of anterior calculi would be contraindicated. Reverting to more invasive interventions, however, may be prevented by carefully selecting patients for Foley extraction.
Our novel technique facilitated manipulation and TRUS-guided extraction of a posterior urethral stone in the office setting without anesthesia, radiation, trauma to the urethra, or long-term sequelae. Given the advantages of this procedure in contrast to traditional modalities, future studies are needed to determine if TRUS-guided Foley extraction should become a first-line method to manage non-impacted small- to medium-sized urethral calculi, regardless of shape, in patients with favorable anatomy and without significant intraprostatic calcifications that preclude safe identification of the stone. Our technique is relatively contraindicated in situations where the urethra is more susceptible to trauma, including patients with urethral stricture, urethral diverticulum, or large stones. The placement of an indwelling Foley catheter for a few days is optional.
Conclusions
Our proposed use of real-time TRUS is a novel modality in the diagnosis and treatment of an obstructing stone located in the prostatic urethra. Advantages of TRUS versus retrograde urethrography and voiding cystourethrography are that radiation exposure is minimized and calculi can be visualized regardless of radiolucency. With regards to the patient care, this technique facilitated removal of the impacted stone by direct visualization during stone manipulation and extraction in the office setting.
Acknowledgements
The authors are thankful to Drs. Kelly Warren, Todd Miller, and Peter Brink for departmental support, as well as Mrs. Wendy Isser and Ms. Grace Garey for literature retrieval.
Footnote
Conflicts of Interest: The authors have no conflicts of interest to declare.
Informed Consent: Written informed consent was obtained from the patient for publication of this case report and any accompanying images.
References
- Koga S, Arakaki Y, Matsuoka M, et al. Urethral calculi. Br J Urol 1990;65:288-9. [Crossref] [PubMed]
- Sharfi AR. Presentation and management of urethral calculi. Br J Urol 1991;68:271-2. [Crossref] [PubMed]
- Houlgatte A, Fournier R. stones and foreign bodies of the urethra. Ann Urol (Paris) 2004;38:45-51. [Crossref] [PubMed]
- Kamal BA, Anikwe RM, Darawani H, et al. Urethral calculi: Presentation and management. BJU Int 2004;93:549-52. [Crossref] [PubMed]
- Villaume F 4th, Plummer D, Caroon L. Diagnosis and removal of urethral calculi using bedside ultrasound in the emergency department. Acad Emerg Med 2009;16:1031-2. [Crossref] [PubMed]
- Mihmanli I, Kantarci F, Gulsen F, et al. Transrectal voiding sonourethrography for diagnosis of a prostatic urethral calculus. J Ultrasound Med 2006;25:1455-7. [Crossref] [PubMed]
- Koh CJ, De Filippo RE, Bochner BH, et al. Extensive bladder and urethral calculi detected with computerized tomography: Diagnosis and management. J Urol 1999;162:158. [Crossref] [PubMed]
- Park SJ, Yi BH, Lee HK, et al. Evaluation of patients with suspected ureteral calculi using sonography as an initial diagnostic tool: How can we improve diagnostic accuracy? J Ultrasound Med 2008;27:1441-50. [Crossref] [PubMed]
- Gamal W, Eldahshoury M, Hussein M, et al. Cystoscopically guided percutaneous suprapubic cystolitholapaxy in children. Int Urol Nephrol 2013;45:933-7. [Crossref] [PubMed]
- Al-Ansari A, Shamsodini A, Younis N, et al. Extracorporeal shock wave lithotripsy monotherapy for treatment of patients with urethral and bladder stones presenting with acute urinary retention. Urology 2005;66:1169-71. [Crossref] [PubMed]
- Rizvi SA, Naqvi SA, Hussain Z, et al. Management of pediatric urolithiasis in pakistan: Experience with 1,440 children. J Urol 2003;169:634-7. [Crossref] [PubMed]
- Safwat AS, Hameed DA, Elgammal MA, et al. Percutaneous suprapubic stone extraction for posterior urethral stones in children: Efficacy and safety. Urology 2013;82:448-50. [Crossref] [PubMed]


