Surgical treatment of Peyronie’s disease by modified 16-dot placation in China
Introduction
Peyronie’s disease (PD) is known as the deposition of collagens that creates a fibrous inelastic scar in the tunica albuginea of the penis. Patients with PD typically exhibit any single or combined presentation of penile induration, plaque, curvature, shortening, narrowing, painful erections, and subsequent erectile dysfunction. These various deformities and the associated psychological distress obviously affect the quality of life of both the patient and his partner (1,2). Although several assumptions or hypotheses have been proposed including genetic predisposition, inflammation and trauma during sexual intercourse, the exact etiology or causes of PD is still unclear and thus, it results in difficulty of making an effective therapeutic strategy for PD (1,2).
The progression of PD varies among different individuals. The initial acute phase is often characterized by acute inflammation and painful erection. Although several conservative therapies have been used in this phase, the results of these treatments are often disappointing (2). Although the penile pain usually resolves spontaneously within 6-18 months of PD onset in most patients, curvature and deformities progression will start when the active inflammation ceases. In the chronic phase, surgical treatment options remain as the gold standard for treatment of PD, but it should only be considered after the disease was stabilized (2,3).
Among several surgical techniques, the Lue’s 16- or 24-dot minimal tension plication has yielded satisfactory results in various types and degrees of penile curvature, and has been widely accepted by many surgeons (1,3-5). We evaluated the feasibility of 16-dot plication technique and its modification in China and report our experience in 32 patients with PD during minimum 4-year period.
Subjects and methods
Between August 2004 and December 2008, 32 patients (aged from 20 to 61 years) with PD underwent surgical correction of penile curvature by 16-dot plication and its modification in our institution. PD patients with adequate erectile capacity and any single or combined presentation including a penile angle of greater than 30 degrees, difficulty or inability to allow vaginal penetration for intercourse and painful vaginal penetration were candidates for this surgery, whereas patients with diminished erectile capacity who did not respond to oral pharmacotherapy or intracavernosal injection were recommended penile prosthesis implantation. All patients had stable disease for at least 6-12 months before the surgery. Preoperative evaluation included medical and sexual history with International Index of Erectile Function 5 (IIEF-5) questionnaire, pain on erection, physical examination. The location and degree of curvature during erection were determined by at-home photography by the patients or by artificial erection induced by intra-cavernosal injection of papaverine (30 mg) if the patient was unable to obtain a photograph.
The surgical procedure performed in our study was similar to that described by Gholami and Lue with minor modifications (4). Briefly, the penis was degloved using a circumcision incision and an artificial erection was induced by injection of normal saline solution containing papaverine (Figure 1A). After assessing the degree of deformity and the point of maximal curvature, center of the curvature and four sets of four dots proximal and distal to the curvature were marked. Then two pairs of longitudinal plication were made by 2-zero non-braided polyester sutures through the full-thickness of the tunica albuginea on the opposite site of the center of the curvature. All of the plication sutures avoided disturbing neurovascular structures and the tension of sutures was adjusted until the complete straightening of the penis was confirmed by artificial erection. Eight patients with combined curvatures (dorsal lateral or ventral lateral) and greater curvature more than 60°, the same techniques were used but with 24 (3 pairs) or 32 (4 pairs) dots and widened spaces between the sutures to ensures a minimal tension repair (Figure 1B, C).
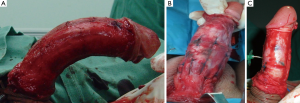
Following surgery, patients were recommended to abstain from all forms of sexual intercourse for two months. In addition, patients were recommended daily low dose phosphodiesterase type 5 (PDE5) inhibitors two weeks after surgery and maintained for two months in order to enhance recovery of erectile function. At follow-up, satisfaction of patient and their partner and erectile function were assessed using IIEF-5 questionnaire at 3-, 6-months, 1 year postoperatively and every 1 year thereafter.
Results
There were no surgery-related complications, such as hematoma, urethral injury, or infection.
All patients were satisfied with postoperative penile length while shortening of the penis was noted in 13 patients (40%), and the median loss of penile length was 1.5 cm (range, 0.8-2.2 cm).
Of patients with plication procedure, 24 patients had penile curvatures within 60° preoperatively. Among these patients, 20 patients reported straight erections, 4 patients complained slight residual curvature but without affection of sexual intercourse at 6-months postoperatively. At 6-months postoperatively, one of the 8 patients with curvature greater than 60° had a recurrence of curvature angle <50° and underwent the same surgical procedure again by using 32 (4 pairs) dots and had excellent results; meanwhile, the other patient primarily underwent surgery by using 32 (4 pairs) dots had no recurrence.
Of all patients, 20 patients had received PDE5 inhibitors two weeks after surgery and maintained for two months. Among these patients, the IIEF-5 score, which showed a significant improvement, increasing from 16.8 (range, 15.5-21.3) to 18.2 (range, 17.6-22.0), 20.9 (range, 19.8-24.3) and 22.6 (range, 20.2-25.8), at 3-, 6- and 12-month follow-up, respectively. One year after surgery, all 20 patients were able to have normal sexual intercourse, and only 20% patients required PDE5 inhibitors to achieve adequate erectile capacity; this percentage increased to 40% after a median follow-up period of 71 months (range, 50-92 months). However, the 12 patients that had not received PDE5 inhibitors after surgery showed slightly lower improvement in IIEF-5 score, which was from 16.9 (range, 15.6-20.7), to 17.6 (range, 16.3-20.7), 19.2 (range, 18.2-21.4) and 20.9 (range, 18.5-23.5), at preoperatively, 3-, 6- and 12-month follow-up, respectively. One year after surgery, 33% patients required PDE5 inhibitors to achieve adequate erectile capacity; the percentage increased to 58% after a median follow-up period of 71 months (range, 50-92 months).
Other complications such as diminished postoperative penile sensation, palpable suture knots and painful erection were noticed in 4 (13%), 8 (25%), 2 (6%) patients, respectively, but these complications did not affect their sexual intercourse.
After the surgery, 94% of patients and 88% of partners reported overall satisfaction in pain or discomfort during intercourse or daily erection, penile length, rigidity of erection, penile sensation and palpable suture knots.
Discussion
Penile curvature and subsequent decrease in sexual function are the major problems in the chronic phase of PD. Although reconstructive surgery has been shown to be the most effective way to correct penile curvature, it is only considered in severe cases that have failed conservative management and have stable curvature for longer than 3-6 months (6). In addition, reconstructive surgeries are usually considered when the curvature is more than 30°, though sexual intercourse is already impeded by the entity of 20° curvature (7). However, it is still unclear which operative technique is optimal for erectile capacity, and no single surgical technique is suitable for all cases of PD.
PD patients with adequate erectile capacity are candidates for reconstructive surgery, including shortening of the convex side and lengthening of the concave side and both procedures have their own set of pros and cons (3,6). Despite lengthening procedures which can avoid penile shortening by straightening the concave side, they may result in less satisfy long-term outcomes, due to significant risks for decrease in erectile function and recurrent curvature caused by extensive incision or excision of the plaque (8,9). Therefore, lengthening procedures are now suggested mainly in patients with severe penile curvatures, and/or narrowing or hourglass deformities (2,6). Nesbit procedure and penile plication are the most common surgical techniques for mild to moderate penile curvatures in PD. Although the success rate of these procedures on penile straightening is similar, Nesbit procedure may result in some surgical complications including hematoma, infection, decreased penile sensitivity and erectile dysfunction due to the opening corpora cavernosa and mobilization of neurovascular bundle or corpus spongiosum (6). Meanwhile, tunica albuginea placation, especially the Lue’s 16- or 24-dot minimal tension placation, is a relatively minimal invasive procedure providing similar results (4). The advantage of this method is that the extensive incision or excision of tunica albuginea is not needed, which benefits patients with better erectile capacity and less surgical complications (4). Therefore, we preferred Lue’s 16- or 24-dot minimal tension plication and its modification in our cases with mild to moderate curvature.
The successful rate of complete penile straightening in our patients was similar to other published study. In a series of 116 PD and 16 congenital penile curvature patients, Gholami and Lue (4) reported a 96% rate of satisfaction and a 93% rate of completely straight penis, and the rate of recurrent curvature was 15%. In our study, the recurrence of penile curvature occurred in patient with curvature angle more than 60° and underwent the plication by using 24 (3 pairs) dots. Nevertheless, reoperation with 32 (4 pairs) dots showed excellent results. Meanwhile, the other patients received primary 32 (4 pairs) dots had no recurrence. Therefore, increasing the number of pairs of sutures for a minimal tension is one of the important prerequisite for prevention of recurrence.
Penile shortening is one of the most common side effects of the plication procedures, therefore this procedure is usually recommended to the patients with adequate penile length and penile curvatures within 60° (3,6). Although penile shortening occurred in 40% of our cases, none of patients stated their sexual activity affected by loss of penile length. Nonetheless, two patients in our study had complained the about 2 cm shortening in the first follow-up, but were satisfied with quality of sexual life in the long-term follow-up. Although penile shortening rarely results in intercourse difficulty (10), this side effect must be clearly explained to the patients prior to the surgery.
According to the literature, the plication procedure usually does not affect erectile function (1,4). In our study, this surgery showed a positive effect on erectile function evidenced by IIEF-5 scores. Interestingly, in the surgical process we found that the most patients with PD had thinner or weaker tunica albuginea. Since daily low dose PDE5 inhibitors have beneficial effects on postoperative rehabilitation following penile reconstruction through nourishment and prevention of fibrosis in the healing cavernosal tissue by enhancement of nocturnal erections (11), all the patients in our study were recommended sildenafil 25 mg nightly for two months beginning two weeks after surgery. The results from this study demonstrate that the administration of sildenafil yields more significant improvement in the erectile rehabilitation.
Other complications such as diminished postoperative penile sensation, palpable suture knots and painful erection were noticed in some patients, but these complications did not affect their sexual intercourse.
Conclusions
Correction of penile curvature using the 16- or 24-dot minimal tension plication and its modification is a simple and safe method to achieve satisfactory results in both cosmetically and functionally. The procedure could be recommended for carefully selected PD patients with penile curvature and adequate erectile capacity instead of other more invasive surgical procedures.
Acknowledgments
Funding: This study was supported by the National Natural Science Foundation of China (NO. 81070544, 81172450, 81202008).
Footnote
Conflicts of Interest: The authors have no conflicts of interest to declare.
References
- Gur S, Limin M, Hellstrom WJ. Current status and new developments in Peyronie’s disease: medical, minimally invasive and surgical treatment options. Expert Opin Pharmacother 2011;12:931-44. [PubMed]
- Hatzimouratidis K, Eardley I, Giuliano F, et al. EAU guidelines on penile curvature. Eur Urol 2012;62:543-52. [PubMed]
- Martinez D, Ercole CE, Hakky TS, et al. Peyronie’s Disease: Still a Surgical Disease. Adv Urol 2012;2012:206284.
- Gholami SS, Lue TF. Correction of penile curvature using the 16-dot plication technique: a review of 132 patients. J Urol 2002;167:2066-9. [PubMed]
- Lee SS, Meng E, Chuang FP, et al. Congenital penile curvature: long-term results of operative treatment using the plication procedure. Asian J Androl 2004;6:273-6. [PubMed]
- Kadioglu A, Akman T, Sanli O, et al. Surgical treatment of Peyronie's disease: a critical analysis. Eur Urol 2006;50:235-48. [PubMed]
- Syed AH, Abbasi Z, Hargreave TB. Nesbit procedure for disabling Peyronie’s curvature: a median follow-up of 84 months. Urology 2003;61:999-1003. [PubMed]
- Kalsi JS, Christopher N, Ralph DJ, et al. Plaque incision and fascia lata grafting in the surgical management of Peyronie’s disease. BJU Int 2006;98:110-4. [PubMed]
- Kim DH, Lesser TF, Aboseif SR. Subjective patient-reported experiences after surgery for Peyronie’s disease: corporeal plication versus plaque incision with vein graft. Urology 2008;71:698-702. [PubMed]
- Savoca G, Trombetta C, Ciampalini S, et al. Long-term results with Nesbit’s procedure as treatment of Peyronie’s disease. Int J Impot Res 2000;12:289-93. [PubMed]
- Levine LA, Greenfield JM, Estrada CR. Erectile dysfunction following surgical correction of Peyronie’s disease and a pilot study of the use of sildenafil citrate rehabilitation for postoperative erectile dysfunction. J Sex Med 2005;2:241-7. [PubMed]


