
Efficacy and safety of novel low-intensity pulsed ultrasound (LIPUS) in treating mild to moderate erectile dysfunction: a multicenter, randomized, double-blind, sham-controlled clinical study
Introduction
Erectile function requires coordinated interaction of multiple organ systems include psychological, endocrine, vascular, neurologic regulation. Erectile dysfunction (ED) is a common disease, which affects more than 50% of men between the ages of 40 and 70 years (1). In 2010, a report from the European Male Ageing Study (EMAS) has illustrated that one third of men (prevalence of 30–64%) in their population were dissatisfied with their overall erectile function or sexual relationship (2). Studies indicated that more than 50% ED showed organic causes due to cardiovascular disease, diabetes mellitus, trauma or surgery on colon, bladder, prostate, genitourinary, neurologic causes (lumbar disc, MS, CVA), Priapism, hormone deficiency et al., which could induce corpus cavernosum pathological changes include corpus cavernosm smooth muscle apoptosis and fibrosis, endothelial dysfunction neuropathy et al.
Currently, the first line ED therapeutic approach is phosphodiesterase type 5 inhibitors (PDE5is). And the second line choices include intracavernosal injection therapy, vacuum devices used for treating mild to moderate ED patients once a time symptom treatment, and the first line and second line therapies no responder severs ED patients need to be treated by penile prostheses implantation surgery (3,4). The most obvious limitation of all these above-mentioned therapies is symptomatic treatment and could not restore the pathological changes in erectile tissue significantly.
Although some of alternative therapies for ED have been extensively reported recently, including exogenous stem cell therapy, gene therapy, and tissue engineering et al. in preclinical studies, however, there is still needed long-term investigation before real clinical approach due to ethic, immunological problem, limited efficacy and safety problems (5-9). Very recently, low energy shock wave therapy (LESWT), a form of physical therapy in micro-energy therapy, was shown to significantly improve erectile function both in animal studies and clinical settings (9,10).
A micro-energy related therapy for the management of ED represents a typical model of convergence science of life science, physical sciences, and engineering. Another important form of energy medicine in the field of translational medicine is low-intensity ultrasound. Ultrasound with acoustic frequencies in excess of 20,000 Hz has traditionally been used in imaging medicine. However, since 1927, its biological effects have also been extensively explored (11). Low-intensity pulsed ultrasound (LIPUS) is a form of pulse ultrasound that is delivered at an intensity lower than 3 W/cm2. The energy is delivered in a pulsed fashion to reduce the thermal effect of ultrasound that might induce local tissue damage. Previous studies have demonstrated that LIPUS has beneficial effects for connective tissue regeneration, inflammation control, and neovascularization (12-16).
The novel device of LIPUS therapy device for ED was developed by Beijing Wanbeili Medical Instrument Co., Ltd., and cooperated with the Molecular Biology Laboratory, Andrology Center of Peking University First Hospital, and the Knuppe Molecular Urology Laboratory of University of California, San Francisco. The novel ultrasound pulse duration - pulse interval ratio is 1:4 (200 µs:800 µs) at 1,000 Hz and frequency of 1.7 MHz. In our previous study, this LIPUS therapy improved the pathological changes in penile erectile tissue of streptozotocin (STZ)-induced diabetic rats and enhanced erectile function [intracavernous pressure (ICP)], increased endothelial and smooth muscle content, increased expression of eNOS and nNOS, and decreased collagen and fiber changes with down-regulation of TGF-β1/Smad/CTGF signaling pathway. No treatment-related adverse events (AEs) were found in animal studies (9).
In order to investigate the efficacy and safety of LIPUS in the clinical treatment of patients with ED, a multicenter, randomized, double-blind, sham-treated, controlled clinical study was conducted.
Methods
Patients’ recruitment
Patients were recruited in 5 centers (Peking University First Hospital, Beijing, China; Affiliated Hospital of Weifang Medical University, Weifang, Shandong, China; Lanzhou University Second Hospital, Lanzhou, Gansu, China; The First Affiliated Hospital of Zhengzhou University, Zhengzhou, Henan, China; Beijing Chaoyang Hospital, Beijing, China). The inclusion criteria and exclusion criteria were summarized in Table 1. Because there was no previous report on LIPUS treatment, the case number was calculated based on the hypothesis that the effective rate is 70% in treatment group and 40% in control group. The α was set as 0.05 (two tail) and the ratio of case number in treatment group to control group was 2:1. In order to reach a test power of 80%, 93 cases (62 cases in treatment group and 31 cases in control group) were needed. We hypothesis the dropout rate was 20%, and final recruited case number was set as 120 (80 in treatment group and 40 in control group). The entire procedure was approved by China Food and Drug Administration (CFDA, Chinese Clinical Trial Registry: ChiCTR1800018954) and Ethics Committee of each hospital (Table 2). Informed consent was obtained from each recruited patient.
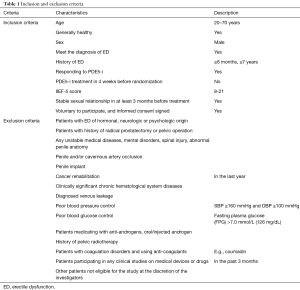
Full table
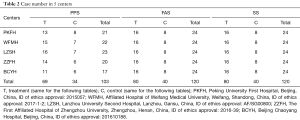
Full table
Intervention
Before the first treatment, a four-week wash out period was applied to all the patients to exclude any potential affection of previously received medication. The treatment lasted for 4 weeks, and patients received LIPUS treatment twice a week. LIPUS was delivered by an adjustable Low intensity pulsed ultrasound therapeutic device (WBL-ED, Wanbeili Medical instrument Co., Ltd, Beijing, China) with a pulse duration time-to-pulse rest time ratio of 1:4 (200 µs:800 µs) at 1,000 Hz and frequency at 1.7 MHz. The I-SATA (spatial average, temporal average intensity) energy intensity levels applied to the patients of control group and treatment group were 0 and 300 mW/cm2 respectively. The sound and vibration of the head of the control machine is designed to be similar to that of the treatment machine. Ultrasound gel was applied to the treatment area to induce intimate contact between penile skin and device. The treatment areas include left crus, right crus, left corpus cavernosum, and right corpus cavernosum. Each session lasted for 20 min in total with 5 min per area. Evaluation and follow up were conducted as the Table 3.
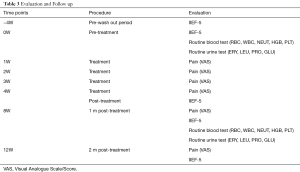
Full table
Evaluation
The primary index for effectiveness is International Index of Erectile Function-5 (IIEF-5). Positive response was defined as [IIEF-5 (12W)]-[IIEF-5 (0W)] ≥2 points. Secondary indexes for effectiveness evaluation include: Sexual Encounter Profile (SEP)-questionnaires 2/3, Global Assessment Question (GAQ), and Erectile Hardness Score (EHS). For safety evaluation, all the AEs and adverse reaction were recorded including: pain [Visual Analogue Scale/Score (VAS)], local petechia or ecchymosis, hematuria and other AEs. Routine blood test (RBC, WBC, NEUT, HGB, PLT) and routine urine test (ERY, LEU, PRO, GLU) were also conducted pre-treatment and 1 month post treatment to detect potential biochemical changes in body fluids.
Statistical analysis
Full analysis set (FAS) includes qualified cases and dropout cases. The patient had been evaluated at least once during the trial. Intention to treat (ITT) analysis was used for data-carry-forward when the value of primary index for effectiveness was missing. Per protocol set (PPS) (PP analysis) includes only qualified cases (Met the inclusion criteria but not the exclusion criteria) with complete case report form (CRF). Security data set (SS) includes cases that received at least one time of treatment and had security records. Part of the cases meeting the exclusion criteria might be included to the SS. SS was used to calculate incidence of AEs and adverse reaction.
The results were analyzed using SAS (v9.4) software and expressed as percent or mean plus or minus standard deviation. Continuous variables of multiple groups were described and compared using t-test or Wilcoxon test (two tailed). The categorical variables were compared between groups using Chi-square test or Fisher’s test. Ranked data was compared using Cochran Mantel Haenszel (CMH) test. Statistical significance was set at P<0.05.
Results
Case description
The total inclusion cases are 120 (treatment 80; control 40) and the number of dropout cases is 17 (11 in treatment group and 6 in control group). All the cases in 5 centers were summarized in Table 2. As for the analysis, FAS was set as 120 (treatment 80; control 40), PPS was set as 103 (treatment 69; control 34) and SS was set as 120 (treatment 80; control 40).
Pre-washout and pre-treatment information
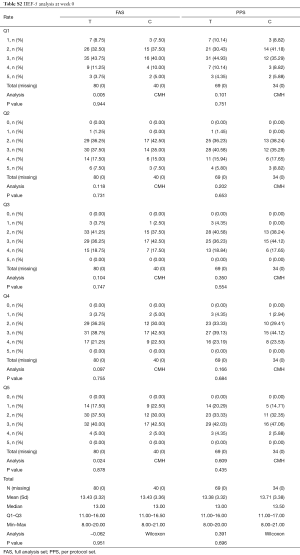
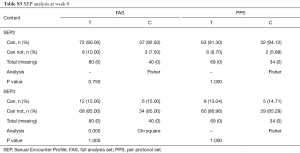
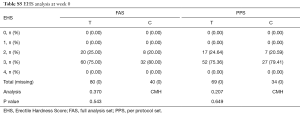
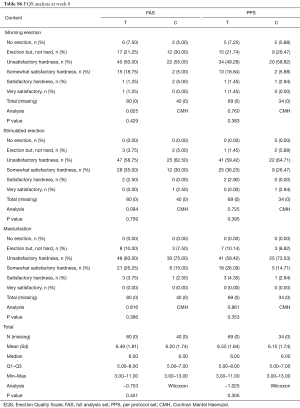
The baseline parameters (age, weight, height, ethnicity, marital status, allergy, smoking, medical history and related treatment) of both groups showed no significant difference. The vital signs (heartbeat, pulse, temperature, blood pressure, respiratory rate) were measured at pre-washout time point (−4W). IIEF-5 was measured at pre-washout and pre-treatment time points (−4W and 0W). No significance was detected (P>0.05) between control and treatment groups. SEP, GAQ, EHS and Erection Quality Scale (EQS) information that were collected at time point 0W also showed no significant difference between two groups (Tables S1-S6).
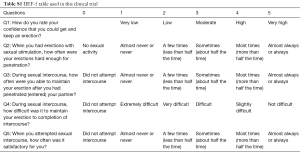
Full table
Full table
Full table

Full table
Full table
Full table
LIPUS treatment improves ED based on the post-treatment IIEF-5 scores
Response rates (increase ≥2 points) were calculated at 4W, 8W, and 12W post-treatment. In the positive responsive category, we further calculate the percentage of patients with an increase of IIEF-5 score more than 3 points or 4 points. In control group, the response rates were 20.59%, 20.59%, and 17.65% at the 3 time points (PPS); while in treatment group, the corresponding response rates were 76.81%, 75.36%, and 71.01% (PPS). The differences were significant (P<0.05, Tables 4 and 5, Figure 1). The average increase of IIEF-5 score in both groups (treatment vs. control) were 3.03±2.06 vs. 1.12±1.49 (4W), 3.35±2.31 vs. 0.71±1.51 (8W), and 4.29±3.20 vs. 0.91±1.11 (12W) (P<0.05, Figure 1).
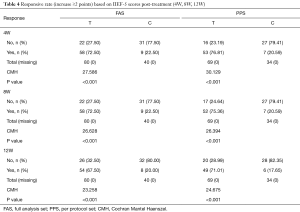
Full table
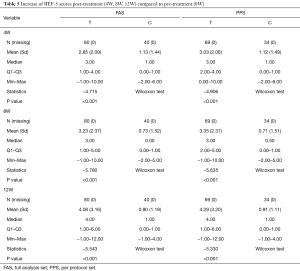
Full table
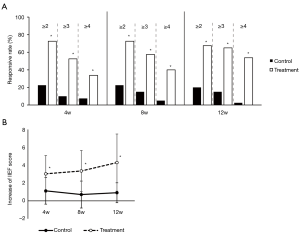
Complementary evaluation indexes regarding to erection improvement
In order to evaluate the erectile function improvement roundly, we further collect and analysis the data of EHS, SEP-questionnaires 2/3, and GAQ-questionnaires 1/2. CMH test of EHS score (Ranked data) revealed that significant change did happen between control and treatment groups 12W after treatment (P=0.012 for FAS analysis and PPS analysis, Table 6). As for SEP-2 (successful vaginal insertion w/o poor erectile rigidity), there were no significant differences between control and treatment groups 4, 8, or 12 weeks post treatment. The percentage of patients with positive answers to SEP-3 (successful/satisfactory vaginal intercourse) were 58.97%, 64.1%, and 73.08% 4, 8, and 12 weeks after treatment which were significantly higher than 28.95%, 31.58%, and 28.95% respectively in control group (FAS, P<0.05). The positive responsive rates for GAQ (“Did the treatment improve your erections” for GAQ1 and “Did the treatment improve your sexual life” for GAQ2) in treatment group were about 2 to 3 times of that in control group (P<0.05, Figure 2).

Full table
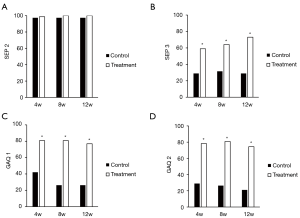
AEs assessment
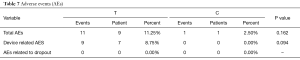
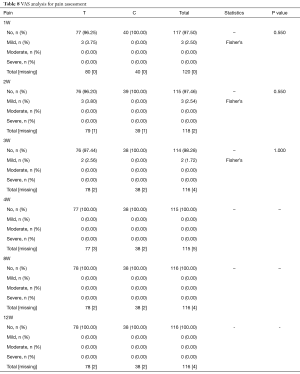
All the AEs were recorded including urinary tract infection (UTI), abscess, local burning feeling, and local pain. The number of device related AEs in treatment group was 9 (happened to 7 patients). No device related AEs were recorded in control group. Local pain was most common recorded AE during the trial. We did the VAS analysis for pain assessment from 1W after treatment to 12 weeks after treatment. No significant difference was founded between control and treatment groups (Tables 7 and 8).
Full table
Full table
Discussion
Although some of alternative therapies for ED have been extensively reported recently, including the exogenous stem cell therapy, gene therapy, and tissue engineering in preclinical studies, however, long-term investigation is still needed before clinical approach due to ethic, immunological problem, limited efficacy, and safety issues (5-9).
Extracorporeal shock wave (ESW) treatment of kidney stone disease is a major revolution in energy therapy. In 2012, the clinical efficacy of low energy shock wave therapy (LESW) for ED was introduced. Our previous studies have shown that LEWS treatment can restore the pathological changes of erectile tissue, and pre-clinical studies have shown that LESW treatment can restore erectile function. The ultrasound and other energy sources of ultrasound have been used for medical purposes more than 70 years, including diagnosis and treatment (17). Ultrasound is defined as sound waves with frequencies above the human hearing threshold and is clinically divided into two main categories, imaging ultrasound and therapeutic ultrasound. Preclinical and clinical studies have shown that LIPUS stimulates tissue regeneration by transmitting mechanical energy. These effects are biomechanical conduction caused by micro-turbulence caused by intercellular and intracellular fluids in the vicinity of the ultrasonic vibration structure. Recently, developments in the science of ultrasound have improved and made ultrasound a possible therapy for various diseases.
Our previous studies (9) have shown that that a continued wave form of low intensity ultrasound showed significant thermal effects that may induce tissue damage-related AEs, and ideal frequency and intensity and pulsed form of LIPUS may significantly reduce thermal effects to improve erectile function with restoring pathological changes in corpus cavernosum of diabetic ED rat model (9). The therapeutic effects of LIPUS were reported in bone disease, wound healing, inflammation, chronic myocardial ischemia et al. However, there are no reports on treatment of ED (12-18).
The novel device of LIPUS for ED was developed by Wanbeili Medical Instrument Co., Ltd., Beijing, China with a pulse duration time-to-pulse rest time ratio of 1:4 (200 µs:800 µs) at 1,000 Hz and frequency at 1.7 MHz. In our previous preclinical study, LIPUS therapy improved erectile function and reversed pathologic changes in penile tissue of STZ induced diabetic rats which were evidenced by enhanced intracavernous pressure (ICP) level, increased endothelial and smooth muscle content, increased eNOS and nNOS expression and modified collagen and fiber changes with downregulation of TGF-β1/Smad/CTGF signaling pathway (9). No treatment related AEs were found in animal studies. With promising results of Low intensity pulsed ultrasound (LIPUS) therapy from our preclinical animal studies (9).
The therapeutic biological effectiveness of ultrasonic therapy is influenced by its application parameters such as intensity, frequency, continuous/pulsed current, and time of irradiation. In this clinical trial, the parameters of LIPUS treatment (1:4, 1,000 HZ, 300 mW/cm2) were chosen based on data from previous animal studies and LESW studies (9,18). Patients received treatment once a week for 4 weeks and each session lasting a total of 20 minutes, with each treatment area lasting 5 minutes.
The underlying mechanisms of LIPUS are still not fully understood. Previous studies of LIPUS have focused on promoting fracture healing, accelerating soft tissue healing, inhibiting inflammatory responses, and controlling pain and musculoskeletal function recovery (19). Cruz et al. reported that ultrasound treatment of 1 MHz continuous (0.4 W/cm2 SATA) or pulse (20% duty cycle, 0.08 W/cm2 SATA) was found to improve endothelial function in humans and has an anti-inflammatory effect (20). According to Watson, the overall effect of ultrasound in damaged tissue is pro-inflammatory, which leads to tissue repair (21-23). In our previous animal study, LIPUS therapy has been shown to significantly improve erectile function in diabetic rat models, as evidenced by increased ICP levels, increased endothelial and smooth muscle content, and increased eNOS and nNOS expression (9).
In most clinical settings, physical therapies including LIPUS and LESW are conducted in a chronic way, in which patients receive therapy once or twice a week for four to eight weeks (24-27). The treatment protocol is corresponding to the tissue rehabilitation speed such as nerve regeneration. Although no treatment related AEs were recorded in our animal studies and clinical tries, we have no long-term safety evaluation of LIPUS treatment by now.
For evidence based clinical study, a multicenter, randomized, double-blind, shame controlled clinical trial was performed in this study and our results for the first time in clinical setting illustrated that LIPUS is beneficial for the treatment of mild to moderate ED.
Inclusion criteria in this study we select mild to moderate ED patients for Ideal results and due to LIPUS without noise like ESWT, we add vibratory sensation in both of shame control group and LIPUS treatment group for double blind study. In the present clinical trial, we found that LIPUS has similar effects with previously reported LESW on treating mild to moderate ED patients (18,25,28). LIPUS and LESW are both falling into the category of mechanical stimulus, however, they have very different physical properties. The energy output is more stable for LIPUS. LIPUS wave transmits mechanical energy by perturbing cells around their equilibrium position (29). It is believed that a non-traumatic mechanical stimulus might triggers cellular deformation and induce extra cellular matrix (ECM)-cytoplasm signal transduction (30,31). Signals transmit to nucleus finally go through cytoskeleton (actin) resulting more subsequent responses by modified gene expression including inflammatory molecules such as IL-1 and IL-6, and neural growth-related factors such as BDNF (32). Fan et al. even found the effect of acoustic actuation of integrin-bound microbubbles for mechanical phenotyping during differentiation of stem cells (33). In their study, functionalized microbubbles targeted to integrin are employed for in situ measurement of cell stiffness during human embryonic stem cell (hESC) differentiation and morphogenesis. Cell stiffness which remains unchanged in undifferentiated hESCs, is significantly increased during neural differentiation. Ultrasound therefore provides a versatile platform for in situ measurement and manipulation of cellular mechanical property, cell differentiation and cell fate. As for ED treatment, the mechanical signals illustrated by LIPUS or LESW transmitted to the local tissue cells induce extracellular matrix molecular changes and intracellular composition changes. The above-mentioned mechanisms alter the cavernously structure/composition and local micro environment which might be related activation endogenous stem cell to beneficial for local tissue regeneration and rehabilitation (15,16).
In general, LIPUS is a novel noninvasive method and is suited for use in combination therapy to treat ED, such as paired with oral PDE5is. A huge advantage of LIPUS compared to LESW is that, LIPUS can be delivered using a portable system that can be easily applied in the comfort of patients’ homes. Potential LIPUS in the other therapeutic application such as stress urinary incontinence could be expected in the near future.
Conclusions
These results indicate that LIPUS can effectively treat patients with mild to moderate ED without significant AEs, which is related to the mechanical force of LIPUS and can restore the pathological changes within the corpus cavernosum. LIPUS is a promising alternative therapeutic method for ED treatment in the near future and the further study is needed.
Acknowledgments
None.
Footnote
Conflicts of Interest: The authors have no conflicts of interest to declare.
Ethical Statement: The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. The entire procedure was approved by China Food and Drug Administration (CFDA, Chinese Clinical Trial Registry: ChiCTR1800018954) and Ethics Committee of each hospital (Table 2). Informed consent was obtained from each recruited patient.
References
- Campbell JD, Burnett AL. Neuroprotective and Nerve Regenerative Approaches for Treatment of Erectile Dysfunction after Cavernous Nerve Injury. Int J Mol Sci 2017. [Crossref] [PubMed]
- Corona G, Lee DM, Forti G, et al. Age-related changes in general and sexual health in middle-aged and older men: results from the European Male Ageing Study (EMAS). J Sex Med 2010;7:1362-80. [Crossref] [PubMed]
- Hawksworth DJ, Burnett AL. Pharmacotherapeutic management of erectile dysfunction. Clin Pharmacol Ther 2015;98:602-10. [Crossref] [PubMed]
- Ryu JK, Suh JK, Burnett AL. Research in pharmacotherapy for erectile dysfunction. Transl Androl Urol 2017;6:207-15. [Crossref] [PubMed]
- Zhou F, Xin H, Liu T, et al. Effects of icariside II on improving erectile function in rats with streptozotocin-induced diabetes. J Androl 2012;33:832-44. [Crossref] [PubMed]
- Xu Y, Guan R, Lei H, et al. Therapeutic potential of adipose-derived stem cells-based micro-tissues in a rat model of postprostatectomy erectile dysfunction. J Sex Med 2014;11:2439-48. [Crossref] [PubMed]
- Lin CS, Xin Z, Dai J, et al. Stem-cell therapy for erectile dysfunction. Expert Opin Biol Ther 2013;13:1585-97. [Crossref] [PubMed]
- Orabi H, Lin G, Ferretti L, et al. Scaffoldless tissue engineering of stem cell derived cavernous tissue for treatment of erectile function. J Sex Med 2012;9:1522-34. [Crossref] [PubMed]
- Lei H, Xin H, Guan R, et al. Low-intensity Pulsed Ultrasound Improves Erectile Function in Streptozotocin-induced Type I Diabetic Rats. Urology 2015;86:1241.e11-8. [Crossref] [PubMed]
- Hausner T, Pajer K, Halat G, et al. Improved rate of peripheral nerve regeneration induced by extracorporeal shock wave treatment in the rat. Exp Neurol 2012;236:363-70. [Crossref] [PubMed]
- ter Haar G. Therapeutic ultrasound. Eur J Ultrasound 1999;9:3-9. [Crossref] [PubMed]
- Urita A, Iwasaki N, Kondo M, et al. Effect of low-intensity pulsed ultrasound on bone healing at osteotomy sites after forearm bone shortening. J Hand Surg Am 2013;38:498-503. [Crossref] [PubMed]
- Ikai H, Tamura T, Watanabe T, et al. Low-intensity pulsed ultrasound accelerates periodontal wound healing after flap surgery. J Periodontal Res 2008;43:212-6. [Crossref] [PubMed]
- Nakao J, Fujii Y, Kusuyama J, et al. Low-intensity pulsed ultrasound (LIPUS) inhibits LPS-induced inflammatory responses of osteoblasts through TLR4-MyD88 dissociation. Bone 2014;58:17-25. [Crossref] [PubMed]
- Toyama Y, Sasaki K, Tachibana K, et al. Ultrasound stimulation restores impaired neovascularization-related capacities of human circulating angiogenic cells. Cardiovasc Res 2012;95:448-59. [Crossref] [PubMed]
- Hanawa K, Ito K, Aizawa K, et al. Low-intensity pulsed ultrasound induces angiogenesis and ameliorates left ventricular dysfunction in a porcine model of chronic myocardial ischemia. PLoS One 2014;9:e104863. [Crossref] [PubMed]
- Darrow DP. Focused Ultrasound for Neuromodulation. Neurotherapeutics 2019;16:88-99. [Crossref] [PubMed]
- Li H, Matheu MP, Sun F, et al. Low-energy Shock Wave Therapy Ameliorates Erectile Dysfunction in a Pelvic Neurovascular Injuries Rat Model. J Sex Med 2016;13:22-32. [Crossref] [PubMed]
- Santana-Rodriguez N, Clavo B, Llontop P, et al. Pulsed Ultrasounds Reduce Pain and Disability, Increasing Rib Fracture Healing, in a Randomized Controlled Trial. Pain Med 2018. [Epub ahead of print]. [Crossref] [PubMed]
- Cruz JM, Hauck M, Cardoso Pereira AP, et al. Effects of Different Therapeutic Ultrasound Waveforms on Endothelial Function in Healthy Volunteers: A Randomized Clinical Trial. Ultrasound Med Biol 2016;42:471-80. [Crossref] [PubMed]
- Kiraly M, Varga Z, Szanyo F, et al. Effects of underwater ultrasound therapy on pain, inflammation, hand function and quality of life in patients with rheumatoid arthritis - a randomized controlled trial. Braz J Phys Ther 2017;21:199-205. [Crossref] [PubMed]
- Luz MA Junior, Sousa MV, Neves LA, et al. Kinesio Taping(R) is not better than placebo in reducing pain and disability in patients with chronic non-specific low back pain: a randomized controlled trial. Braz J Phys Ther 2015;19:482-90. [Crossref] [PubMed]
- Hashish I, Hai HK, Harvey W, et al. Reduction of postoperative pain and swelling by ultrasound treatment: a placebo effect. Pain 1988;33:303-11. [Crossref] [PubMed]
- Xiang J, Wang W, Jiang W, et al. Effects of extracorporeal shock wave therapy on spasticity in post-stroke patients: A systematic review and meta-analysis of randomized controlled trials. J Rehabil Med 2018;50:852-9. [Crossref] [PubMed]
- Lei H, Liu J, Li H, et al. Low-intensity shock wave therapy and its application to erectile dysfunction. World J Mens Health 2013;31:208-14. [Crossref] [PubMed]
- Clavijo RI, Kohn TP, Kohn JR, et al. Effects of Low-Intensity Extracorporeal Shockwave Therapy on Erectile Dysfunction: A Systematic Review and Meta-Analysis. J Sex Med 2017;14:27-35. [Crossref] [PubMed]
- Lu Z, Lin G, Reed-Maldonado A, et al. Low-intensity Extracorporeal Shock Wave Treatment Improves Erectile Function: A Systematic Review and Meta-analysis. Eur Urol 2017;71:223-33. [Crossref] [PubMed]
- Liu J, Zhou F, Li GY, et al. Evaluation of the effect of different doses of low energy shock wave therapy on the erectile function of streptozotocin (STZ)-induced diabetic rats. Int J Mol Sci 2013;14:10661-73. [Crossref] [PubMed]
- Humphrey VF. Ultrasound and matter--physical interactions. Prog Biophys Mol Biol 2007;93:195-211. [Crossref] [PubMed]
- Miller AD, Subramanian A, Viljoen HJ. Theoretically proposed optimal frequency for ultrasound induced cartilage restoration. Theor Biol Med Model 2017;14:21. [Crossref] [PubMed]
- Guilak F. Compression-induced changes in the shape and volume of the chondrocyte nucleus. J Biomech 1995;28:1529-41. [Crossref] [PubMed]
- Pavlov D, Bettendorff L, Gorlova A, et al. Neuroinflammation and aberrant hippocampal plasticity in a mouse model of emotional stress evoked by exposure to ultrasound of alternating frequencies. Prog Neuropsychopharmacol Biol Psychiatry 2019;90:104-16. [Crossref] [PubMed]
- Fan Z, Xue X, Perera R, et al. Acoustic Actuation of Integrin-Bound Microbubbles for Mechanical Phenotyping during Differentiation and Morphogenesis of Human Embryonic Stem Cells. Small 2018;14:e1803137. [Crossref] [PubMed]


