Insurance coverage of male infertility: what should the standard be?
Introduction
Infertility is defined as the inability to conceive a pregnancy after 12 months of regular, unprotected vaginal intercourse (1). Based on national surveys from 2006–2010, 6.0% of married women aged 15–44 years have infertility and 9.4 percent of men aged 15–44 years have infertility in the US (2). When men and women with infertility are surveyed about infertility evaluations, they report that the male partner did not undergo an evaluation 18 to 27 percent of the time (3), despite recommendations from the American Society of Reproductive Medicine that both partners receive infertility evaluations (4). This discrepancy could be driven by many factors including societal expectations that infertility is driven by the female partner’s reproductive health or increased outreach to females among patient advocacy groups.
The American Medical Association recently endorsed the World Health Organization’s classification defining infertility as a disease (5,6). The American Society of Reproductive Medicine also classifies infertility as a disease because it is a “deviation from the normal function of the reproductive system” (1). Despite agreement across multiple international medical organizations and professional societies, infertility is rarely treated as a disease in most insurance plans. Instead, diagnostic testing and therapeutic interventions for infertility are often excluded services, categorized similar to cosmetic surgery. These exclusions require patients to pay out-of-pocket payments for infertility care, even if the patients receive insurance coverage for other health conditions.
This review article will describe what is known about the current state of insurance coverage for infertility in the United States, including expected out-of-pocket costs if infertility care is not a covered service. Then, we will discuss emerging data about various insurance coverage options offered by some employers, and we will close with a discussion of an ideal coverage policy for infertility care.
Infertility is rarely covered by insurance
The Patient Protection and Affordable Care Act (PPACA) of 2010 was the most recent large federal law to mandate insurance policies. The law enumerates multiple essential health benefits that must be covered by applicable insurance policies, but infertility care is not listed as an essential health benefit (7). The rest of the PPACA is also silent about whether insurance policies should cover infertility care, and insurance laws prior to the PPACA did not comment on coverage for infertility care. This has left infertility coverage decisions to the discretion of employers and individual states.
In 2006, RESOLVE, a national infertility advocacy organization, hired the Mercer Organization to survey larger employers (≥200 employees) about current coverage policies for infertility care. Approximately 1,800 companies were contacted and 931 responded. Of the responding organizations, 63% reported providing insurance coverage for infertility evaluations, 39% provided insurance coverage for medication treatments, and 22% provided insurance coverage for in vitro fertilization (IVF) (8). Thirty five percent excluded all infertility care from their insurance plans. There are several limitations to this survey. First, the study is now over 10 years old. Second, the study only surveyed larger employers with ≥200 employees, and 34% of American are employed by companies with less than 100 employees (9). Third, the survey did not ask specifically about male fertility coverage. Finally, this survey only reflects insurance coverage policies in the employer-sponsored insurance market. Approximately 41% of adults aged 19–64 have health insurance coverage from a non-employer source or are uninsured (10).
At the state level, fifteen legislatures have passed laws mandating the inclusion of coverage for infertility evaluations and/or treatments for certain insurance plans (11). Each of the fifteen state laws is unique in terms of its scope of coverage and applicability (Table 1) (11,12). For example, in Massachusetts, coverage requirements apply to all insurance carriers and cover both IVF and diagnosis and treatment of male infertility, including sperm procurement. In Arkansas, insurance mandates do not apply for HMO plans and there is no mention of coverage for male infertility evaluations and/or treatments. Interestingly, despite both sperm and eggs being required for conception, only 8 of the 15 states with state laws mandating insurance coverage for infertility have legislative language that mentions the male partner (11). It is unknown what impact these exclusions may have on couples’ infertility care. It’s possible that men will be less likely to receive needed infertility evaluations if their care is not a covered service. Excluding the male partner leaves the burden of reproductive care on the female partner and risks missing important reversible or irreversible male health conditions.
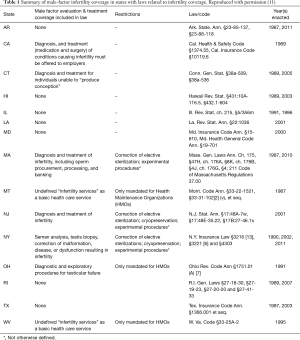
Full table
Infertility care is expensive
Because infertility care is not a covered benefit in most insurance plans, receiving infertility care is often very expensive for patients. In a 2011 study, researchers at University of California, San Francisco followed 391 women for 18 months while they were undergoing evaluations and treatments for infertility. Using standardized costs, they estimated than women receiving infertility evaluations encountered average costs of appropriately $903. Women receiving medication treatment had average costs of $1,403, while intrauterine insemination (IUI) costed patients $7,704 and IVF costed $30,274 (13). A follow-up study asked 332 couples to complete actual cost diaries as they underwent 18 months of male and female infertility evaluations and treatments. This study found that average out-of-pocket costs were $912 for receiving medications alone, $2,623 for receiving IUI, and $19,234 for receiving IVF. Being college-educated and having higher incomes were associated with increased spending (14).
Finally, research from Elliott and colleagues was able to estimate the out-of-pocket expenses associated with male infertility evaluation and treatment. The research team asked 111 men pursuing infertility care to complete cost questionnaires at the culmination of their therapies. Sixty four percent of men reported spending greater than or equal to $15,000, while 16% of men reported spending greater than or equal to $50,000. On average, men reported spending 16–20% of their annual incomes on infertility-related expenses with 47% experiencing financial strain and 46% having treatment options limited by costs (15). It’s worth noting that these studies were performed in the San Francisco area, an area with greater than average annual incomes. According to the U.S. Bureau of the Census, the 2016 national median household income was $59,039 (16).
The impact of insurance coverage for infertility care
As mentioned previously, 15 states have mandated that some or all insurance plans within the state offer or provide coverage for infertility care (17). Research from these states has shown that states with insurance mandates that cover IVF or other fertility treatments perform more IVF cycles per 1,000 women of reproductive age (12), more IUI cycles (18), and more hybrid (18) cycles compared to states without such mandates. Importantly, in states with mandated IVF coverage, there are also less embryos transferred per cycle, a lower percentage of live births per cycle, and a lower rate of multiples per cycle due to embryo-transfer guidelines placed on covered IVF cycles (12).
Embryo-transfer guidelines are an important part of the insurance mandates. When couples are paying out-of-pocket for expensive services such as IVF, there is an understandable desire to maximize the chance of having a live birth with each cycle. This often means transferring more than one embryo which, while increasing the chance of a life birth, also increases the chance of having a multiple gestation (19). Multiple gestations put the mother and baby at increased risk of adverse outcomes, including premature birth. If the child requires time in the neonatal intensive care unit (NICU) or other interventions, health care costs are also increased (19).
Unfortunately, there have been no studies on the impact of mandated infertility insurance coverage on male infertility evaluations and treatments. As noted above, 7 of the 15 states with female infertility mandates do not include any coverage for the male partners.
Why access to male infertility care matters
Both the American Society of Reproductive Medicine (20) and the National Institute for Health and Care Excellence in the United Kingdom (21) recommend that infertile couples begin their evaluations together. These recommendations exist for several reasons, most notably because male infertility is the main cause a couple’s inability to conceive in approximately 30% of cases and contributes to the cause of infertility in addition 20% of cases (22). Insurance coverage for, and access to, male infertility care is important to:
- Identify and correct reversible causes of male infertility;
- Identify irreversible conditions that may be amenable to assisted reproductive technologies;
- Identify irreversible conditions not amenable to assisted reproductive technologies;
- Identify medical diseases associated with male infertility;
- Identify genetic conditions that may be transmitted to offspring.
If men lack insurance coverage for infertility care, they will be less likely to present for initial evaluations due to the expected out-of-pocket expenses, and male infertility has been associated with other significant health conditions. In a retrospective review of 536 male infertility evaluations at 2 academic medical centers, 33 patients (6%) were found to have significant other pathology identified during the evaluation including cases of testicular cancer, prostate cancer, diabetes mellitus, hypothyroidism, cystic fibrosis, and chromosomal abnormalities (23).
Moreover, epidemiologic studies have found that male infertility is associated with increased cardiovascular risk among childless men (24), increased risk of developing testicular cancer (25,26), a 2.6 times increased likelihood of being diagnosed with high grade prostate cancer (27), increased risk of multiple cancers in azoospermic men (28), and increased mortality among men with poorer sperm quality (29,30). Obesity is also associated with reduced sperm quality (31), and weight loss may help improve sperm quality (32).
Finally, male infertility treatments can downgrade the intensity of interventions required for the couple to achieve a pregnancy (33). Therefore, without insurance coverage for—and access to—male fertility care, the burden for reproductive care is left for the female partner. This exposes the female partner to potentially avoidable additional testing, medications, and invasive treatments. To receive her care, the female partner will also have to take time away from work, school, or other commitments at home.
Emerging patient-reported insurance coverage data
Recently, new data has emerged about infertility insurance coverage from certain employers. FertilityIQ is a company from San Francisco that collects patient-reported data on female infertility evaluations and treatments. In addition, FertilityIQ has begun collecting information about infertility coverage options from large companies across multiple sectors. They released their recent report on employer-sponsored coverage of infertility benefits in 2017, which was based on data from over 10,000 patients who underwent IVF in the US (34). The report details many important findings. First, 63% of patients receiving IVF had zero insurance coverage for their cycle while 20% of patients reported complete or near complete coverage. Among a 200-person subset of the women who had complete IVF coverage, 88% of women who delivered a baby returned back to the same employer after maternity leave and 62% reported being more likely to remain in their jobs for a longer period of time.
Insurance coverage of male infertility: What should the standard be?
Given that infertility is a disease, infertility is common, infertility care is expensive, state insurance laws mandating infertility coverage are rare and typically exclude male-factor coverage, and access to fertility care is facilitated by insurance, what should the standard be for insurance coverage for male fertility services?
At a minimum, because infertility is a disease, insurance coverage for evaluations and treatments should mirror coverage for other diseases like diabetes, glaucoma, and cancer. In fact, studies have found that being diagnosed with infertility has a similar psychological impact on patients as being diagnosed with cancer (35).
More specifically, insurance coverage for male fertility care should include coverage for medically indicated diagnostic testing including evaluation and management visits, laboratory tests including hormonal and genetic testing, semen analyses including advanced testing such as DNA fragmentation testing and fluorescence in situ hybridization testing, and diagnostic testicular biopsies. The standard for therapeutic coverage should include indicated medications, including off-label use of established, safe, and efficacious medications such as clomiphene, anastrozole, human chorionic gonadotropin, and recombinant follicular stimulating hormone. In addition, therapeutic coverage should include surgical therapies such as microsurgical varicocelectomy, electroejaculation, penile vibratory stimulation, testicular and epididymal sperm retrieval, and microsurgical testicular sperm extraction. Therapeutic coverage should also include sperm banking for men about to receive gonadotoxic therapies as a means of preventing future infertility. Standard diagnostic and therapeutic interventions for female fertility are beyond the scope of this paper.
Many employers are concerned that covering infertility care would be expensive and drive up insurance premiums (8). Older studies attempted to address this issue. Since 1989, Massachusetts has mandated that all insurance plans provide coverage for IVF (12). A 1997 analysis of statewide data from 1986 to 1993 found that mandated coverage for IVF was associated with a $1.71 increase in per member per month expenditures (36). Separately, a claims-based analysis from a company with approximately 28,000 employees found that there were hidden costs of tests or procedures associated with infertility care, even if the company’s health insurance plan did not cover infertility itself. These hidden costs were estimated at $0.27 to $0.50 per member per month (37). Unfortunately, none of these studies separated the costs associated with covering male verses female infertility care. Most recently, our research team at the University of Michigan is studying the impact that insurance coverage for infertility care has on access to care, quality of care, and costs.
Conclusions
There are multiple reasons why insurance coverage for male infertility is important, not least of all because infertility is a disease and therefore should have insurance similar to other diseases. Without insurance coverage, men will have less access to care and will be more likely to miss opportunities to receive interventions that can downgrade the intensity of treatments needed to achieve a pregnancy. Men will also miss opportunities to identify underlying health conditions associated with infertility. Ideal insurance coverage for male infertility care would cover comprehensive diagnostic testing and treatments indicated to evaluate and treat the infertile man.
Acknowledgements
None.
Footnote
Conflicts of Interest: The author receives grant funding from Blue Cross Blue Shield of Michigan for other work.
References
- Practice Committee of the American Society for Reproductive Medicine. Definitions of infertility and recurrent pregnancy loss. Fertil Steril 2008;89:1603. [Crossref] [PubMed]
- Chandra A, Copen CE, Stephen EH. Infertility and Impaired Fecundity in the United States, 1982-2010: Data from the National Survey of Family Growth. National Health Statistics Reports, No.67. Hyattsville, MD: National Center for Health Statistics. 2013.
- Eisenberg ML, Lathi RB, Baker VL, et al. Frequency of the male infertility evaluation: data from the national survey of family growth. J Urol 2013;189:1030. [Crossref] [PubMed]
- Practice Committee of American Society for Reproductive Medicine. Optimal evaluation of the infertile female. Fertil Steril 2006;86:S264-7. [Crossref] [PubMed]
- Berg Sara. “AMA backs global health experts in calling infertility a disease.” AMA Wire. June 13, 2017. Available online: https://wire.ama-assn.org/ama-news/ama-backs-global-health-experts-calling-infertility-disease. Accessed March 14, 2018.
- Zegers-Hochschild F, Adamson GD, de Mouzon J, et al. International Committee for Monitoring Assisted Reproductive Technology (ICMART) and the World Health Organization (WHO) revised glossary of ART terminology. Fertil Steril 2009;92:1520-4. [Crossref] [PubMed]
- Patient Protection and Affordable Care Act. 42 USC. §18001 et seq. 2010.
- Mercer Health and Benefits. Employer experience with, and attitudes toward, coverage of infertility treatment. Mercer Health and Benefits. 2006. Available online: http://familybuilding.resolve.org/site/DocServer/Mercer_-_Resolve_Final_report.pdf. Accessed March 14, 2018.
- US Small Business Administration. “United States Small Business Profile, 2016.” US Small Business Administration Office of Advocacy. 2016. Available online: https://www.sba.gov/sites/default/files/advocacy/United_States.pdf. Accessed March 14, 2018.
- Kaiser Family Foundation. “Health Insurance Coverage of Adults 19-64: 2016.” Kaiser Family Foundation. Available online: https://www.kff.org/other/state-indicator/adults-19-64/. Accessed March 14, 2018.
- Dupree JM, Dickey RM, Lipshultz LI. Inequity between male and female coverage in state infertility laws. Fertil Steril 2016;105:1519-22. [Crossref] [PubMed]
- Jain T, Harlow BL, Hornstein MD. Insurance coverage and outcomes of in vitro fertilization. N Engl J Med 2002;347:661-6. [Crossref] [PubMed]
- Smith JF, Eisenberg ML, Glidden D, et al. Socioeconomic disparities in the use and success of fertility treatments: analysis of data from a prospective cohort in the United States. Fertil Steril 2011;96:95-101. [Crossref] [PubMed]
- Wu AK, Odisho AY, Washington SL, et al. Out-of-pocket fertility patient expense: data from a multicenter prospective infertility cohort. J Urol 2014;191:427-32. [Crossref] [PubMed]
- Elliott PA, Hoffman J, Abad-Santos M, et al. Out of pocket costs of male infertility care and associated financial strain. Urol Pract 2016;3:256-61. [Crossref]
- Federal Reserve Bank of St. Louis. Median Household Income in the United States. Available online: https://research.stlouisfed.org/fred2/series/MEHOINUSA646N. Accessed March 14, 2018.
- RESOLVE. “Coverage by State.” RESOLVE: The National Infertility Association. Available online: https://resolve.org/what-are-my-options/insurance-coverage/coverage-state/. Accessed March 14, 2018.
- Bitler MP, Schmidt L. Utilization of infertility treatments: the effects of insurance mandates. Demography 2012;49:125-49. [Crossref] [PubMed]
- Michigan Department of Health and Human Services. The Michigan Action Plan for Infertility and Assisted Reproductive Technology (ART). Lifecourse Epidemiology and Genomics Division, Michigan Department of Health and Human Services, Lansing, MI June 2017. Available online: http://www.michigan.gov/documents/mdhhs/MiART_FullReport_3.2.18_COMBINED_616266_7.pdf. Accessed March 15, 2018.
- Practice Committee of the American Society for Reproductive Medicine. Diagnostic evaluation of the infertile female: a committee opinion. Fertil Steril 2015;103:e44-50. [Crossref] [PubMed]
- National Institute for Health and Clinical Excellence. Fertility: Assessment and treatment for people with fertility problems. NICE clinical guideline 156. 2013. Available online: http://guidance.nice.org.uk/cg156. Accessed October 21, 2015.
- Thonneau P, Marchand S, Tallec A, et al. Incidence and main causes of infertility in a resident population (1,850,000) of three French regions (1988-1989). Hum Reprod 1991;6:811-6. [Crossref] [PubMed]
- Kolettis PN, Sabanegh ES. Significant medical pathology discovered during a male infertility evaluation. J. Urol 2001;166:178-80. [Crossref] [PubMed]
- Eisenberg ML, Park Y, Hollenbeck AR, et al. Fatherhood and the risk of cardiovascular mortality in the NIH-AARP Diet and Health Study. Hum Reprod 2011;26:3479-85. [Crossref] [PubMed]
- Walsh TJ, Croughan MS, Schembri M, et al. Increased risk of testicular germ cell cancer among infertile men. Arch Intern Med 2009;169:351-6. [Crossref] [PubMed]
- Raman JD, Nobert CF, Goldstein M. Increased incidence of testicular cancer in men presenting with infertility and abnormal semen analysis. J Urol 2005;174:1819-22; discussion 1822.
- Walsh TJ, Schembri M, Turek PJ, et al. Increased risk of high-grade prostate cancer among infertile men. Cancer 2010;116:2140-7. [PubMed]
- Eisenberg ML, Betts P, Herder D, et al. Increased risk of cancer among azoospermic men. Fertil Steril 2013;100:681-5. [Crossref] [PubMed]
- Jensen TK, Jacobsen R, Christensen K, et al. Good semen quality and life expectancy: a cohort study of 43,277 Men. Am J Epidemiol 2009;170:559-65. [Crossref] [PubMed]
- Eisenberg ML, Li S, Behr B, et al. Semen quality, infertility, and mortality in the USA. Hum Reprod 2014;29:1567-74. [Crossref] [PubMed]
- Ramaraju GA, Teppala S, Prathigudupu K, et al. Association between obesity and sperm quality. Andrologia 2018.50. [PubMed]
- Håkonsen LB, Thulstrup AM, Aggerholm AS, et al. Does weight loss improve semen quality and reproductive hormones? Results from a cohort of severely obese men. Reprod Health 2011;8:24. [Crossref] [PubMed]
- Cayan S, Erdemir F, Ozbey I, et al. Can varicocelectomy significantly change the way couples use assisted reproductive technologies? J Urol 2002;167:1749-52. [Crossref] [PubMed]
- FertilityIQ. “The FertilityIQ Family Builder Workplace Index: 2017 – 2018.” FertilityIQ. Available online: https://www.fertilityiq.com/fertilityiq-data-and-notes/fertilityiq-best-companies-to-work-for-family-builder-workplace-index-2017-2018. Accessed March 14, 2018.
- Domar AD, Zuttermeister PC, Friedman R. The psychological impact of infertility: a comparison with patients with other medical conditions. J Psychosom Obstet Gynaecol 1993;14 Suppl:45-52. [PubMed]
- Griffin M, Panak WF. The economic cost of infertility-related services: an examination of the Massachusetts infertility insurance mandate. Fertil Steril 1998;70:22-9. [Crossref] [PubMed]
- Blackwell RE, William M. Mercer Actuarial Team. Hidden costs of infertility treatment in employee health benefits plans. Am J Obstet Gynecol 2000;182:891-5. [Crossref] [PubMed]


