Electroejaculation combined with assisted reproductive technology in psychogenic anejaculation patients refractory to penile vibratory stimulation
Introduction
Anejaculation is the inability to ejaculate despite an erection; this condition occupies 72% of male infertility resulting from sexual dysfunction (1). Spinal cord injury (SCI) is the most common cause of anejaculation (2-5), whereas retroperitoneal lymph node dissection (6), diabetes mellitus (7), multiple sclerosis (8), and sperm retrieval before intensive anticancer therapy (9) are the uncommon ones. Most of the research on anejaculation was conducted mainly in SCI patients, a prominent etiology for anejaculation. One of the less investigated populations is the psychogenic anejaculation (PAE) patients.
PAE also called idiopathic anejaculation is a unique problem, occupying 0.4–0.5% of anejaculation patients (10). Men who suffer from this problem are otherwise healthy and may experience erections and nocturnal emissions but do not experience ejaculation during either coitus or masturbation. The etiology is presently unknown which may be associated with psychological factors. These patients are often embarrassed by their problem and the problem will be more obvious when the couples want a baby (10).
Various options for the treatment of this condition have been described in order to obtain ejaculates (10-15). Penile vibratory stimulation (PVS) is the first-line treatment for PAE, being less invasive than electroejaculation (EEJ) (11). However, the rates of sperm retrieval of PVS are lower than EEJ. Some religions, such as Orthodox and Judaism with a high prevalence of PAE, forbid the use of PVS (10).
Therefore, lots of these infertile couples desirous of fertility had to choose more invasive methods, such as microsurgical epididymal sperm aspiration (MESA) (16), percutaneous epididymal sperm aspiration (PESA) (17) and testicular sperm aspiration (TESA) (18) which are second-line treatments. MESA involves surgical exploration of the epididymis and is associated with surgical trauma and morbidity, including pain, hematoma and infection. Further, subsequent surgery may be more difficult because of adhesion and fibrosis (16,17). Although PESA and TESA are simple local anesthetic procedures, they are associated with complications including chronic pain, epididymal injury, testicular atrophy, bleeding, scrotal hematoma, and scrotal infection (17,18). Furthermore, sperm from these surgical methods were with poor quality, decreased motility and generally need to be combined with in vitro fertilization (IVF) or intracytoplasmic sperm injection (ICSI) techniques which have to face with the need for ovarian stimulation and the cost of IVF or ICSI (16-18).
EEJ has become an accepted form of semen procurement in PAE patients (10,19-23) which has a 70–90% success rate of obtaining a satisfactory semen sample (23). However, there is no study focusing on the treatment of PAE patents who are refractory to PVS treatment. After 6 years of studying the treatments of PAE patients, our research program has gathered data on 20 PVS-refractory patients who collected their semen species via EEJ. In this study, we evaluated fertilization rates when performing intrauterine insemination (IUI) or ICSI in combination with EEJ for PVS-refractory patients.
Methods
Patients
In this retrospective study, we enrolled 20 couples refractory to the PVS who at least were performed twice unsuccessful PVS procedures treated by EEJ and IUI or ICSI for isolated male PAE in our units between 2009 and 2015. The diagnosis of PAE was based on the inability to consciously ejaculate by masturbation or sexual intercourse. All patients had occasional erections and nocturnal emissions. Retrograde ejaculation and ejaculatory duct obstruction were ruled out after examination. Chromosomal karyotype was detected to be 46,XY in all patients. The level of FSH, LH, PRL, T and E2 were within the normal range. Sensory evoked potentials of the penis and electromyography of the pelvic floor were conducted to exclude any neurological disorders. Besides, patients who could not tolerate transrectal operation or anesthesia were excluded from our study.
In all spouses, history, physical examinations and ovulatory status were evaluated, Couples with female factor in addition to male infertility were also excluded in our study. The study protocol was approved by the Departmental Ethics Committee of Tongji Medical College, Huazhong University of Science and Technology.
EEJ procedure
EEJ was done in cases of PVS failure and was performed on the day of the female spouse ovulation or the day before it. The patients were placed in lateral decubitus position. A rectal probe (CGS Electroejaculator, Ratek Instruments, Sydney, Australia) was placed against the prostate after lubrication under spinal anesthesia (anesthesia level T8-S5). The initial electrical stimulation given was 2 V. This value was progressively increased by 1 to 2 V every 6 to 10 s until the ejaculation occurred. Meanwhile, the assistant collected the semen samples using actions like milking the cows. However, the maximum voltage did not exceed 18 V. The voltage and vital signs of the patients were closely monitored during the entire stimulation. The whole procedure would last 4 or 5 minutes, after that we should check up the rectum by anoscopy. Urine examinations were performed to rule out retrograde ejaculation.
On the first EEJ sessions, all couples were encouraged to consider IUI or sperm cryopreservation.
Monitoring of female ovulation and controlled ovarian hyperstimulation
We monitored the female ovulation through per vagina type-B ultrasonic, and underwent IUI. Or the female partners were super-ovulated and followed by IVF/ICSI (24).
Treatment and analysis of the semen
The total number, concentration, and other parameters were determined by CASA system (WLJY-9000) when the semen was liquefied and incubated for thirty minutes. For sperm cryopreservation, the sample was diluted 1:1 (v/v) in TEST-YOLK buffer with glycerol (14). Aliquots of 0.5 mL were frozen in liquid nitrogen.
Assisted reproductive technology
Choice of treatment with either IUI or ICSI was based on the VCM [volume (mL) × concentration (sperm cells/mL) × percentage progressive motile cells] and patient preference. A VCM lower than 2 was an indication for ICSI. In patients with a higher VCM, IUI was considered (10).
Data collection and statistical analysis
Demographic information was collected for all couples enrolled in our study. The following variables were collected from PAE patients refractory to PVS: semen volume (mL), sperm concentration (millions of sperm per mL ejaculate), sperm motility (percent of sperm with forward progression), assisted reproduction technology (ART) type, No. of treatment cycles and No. of pregnancies.
Statistical analysis was performed using SPSS software (version 12.0; SPSS, Chicago, IL, USA). Results were presented as interquartile range (IQR), and for statistical analysis, the χ2 test was used. Statistical significance was considered at P<0.05.
Results
Participants characteristics
The mean age of the patients was 30 (IQR, 26–36) years. Mean age of the female spouses was 29 (IQR, 24–32) years. All the men suffered from primary infertility of a duration range 6 (IQR, 2–7) years.
Semen analysis
Twenty men underwent a total of 23 procedures of transrectal EEJ, which were all successful. Table 1 reflected the semen characteristics of the total yielded samples.
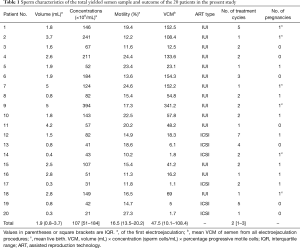
Full table
Result of pregnancy
IUI was performed on 14 couples. Ten of these couples achieved pregnancy in 26 cycles. The overall pregnancy/cycle rate was 38.5%. Five healthy children were born and five pregnancies resulted in spontaneous miscarriage.
A total of 6 couples were treated with 16 cycles of ICSI. Of the 63 oocytes that were injected, 34 (54.0%) were fertilized successfully. The number of implantations was 31, with a pregnancy/implantation rate of 9.7% (3 of 31). The overall pregnancy/cycle rate was 18.8%. One healthy child was born. Two pregnancies resulted in spontaneous miscarriage.
Discussion
Most men with PAE cannot ejaculate by masturbation or coitus and require medical assistance. Psychotherapists can provide treatment for these patients. However, the therapy is of long duration, and the compliance and success rate are rather low (25,26). Thus, PVS and EEJ have been the primary methods of sperm retrieval for PAE couples undergoing assisted conception procedures. PVS is the noninvasive method and first line for PAE patients to obtain their semen. However, there are PAE patients who are refractory to PVS treatment.
EEJ is the most commonly used method to obtain spermatozoa from PAE men which has a up to 90% success rate of obtaining a satisfactory semen sample (23). However, there is no study focusing on these PAE patients who are refractory to PVS treatment. The aim of the study was to evaluate the results of treatment with EEJ, IUI, and ICSI in patients with PAE who were refractory to PVS treatment. In our study, we observed an overall pregnancy/cycle rate of IUI of 38.5%. The total fertilization rate of ICSI was 54.0%. Our pregnancy rate per ICSI cycle was 18.8%. A total of 13 pregnancies were achieved, which resulted in the birth of 6 healthy children.
In our study, all patients ejaculated successfully by EEJ following their failure with PVS. According to the limited literatures, the fertilization and pregnancy rates of ICSI in our study were similar to those reported by Soeterik who evaluated the results of treatment with EEJ, IUI, and IVF/ICSI in patients with PAE, but the pregnancy rate of IUI is higher than that (11.8%, 4 of 34) reported by them (10). The fertilization rate of our study was higher than that (27.5%, 39/142) reported by Hovav (27). A possible explanation for the difference is that all the patients enrolled in our study were PVS-refractory patients. However, there is not an exact definition of PVS-refractory. In our study, these patients received at least two unsuccessful PVS procedures. Another explanation for the observed difference is the higher VCM that we observed in the semen samples. A higher VCM can improve the fertilization rates and, subsequently, may improve the results of assisted reproductive technology.
In our study, most EEJ procedures were safe and could be well tolerated by patients. There was no side effect of rectal injury. However, only one patient displayed the side effect of autonomic dysreflexia in totally 20 patients that underwent 23 EEJ procedures. Consistently, Frankel and Mathias et al. reported that EEJ produced autonomic dysreflexia in men with three SCI patients above T6 (28). However, to confirm whether autonomic dysreflexia was related to the EEJ procedure itself or to the neurologic levels, further study is required.
One thing that should be pointed out is that anesthesia is essential (29). We suggest that the stimulation is given from the minimum voltage of 2 V, and it can be gradually increased 1–2 V per time. The stimulation lasted 6–10 seconds, and one followed another in 15–20 seconds until ejaculation occurred. The maximum voltage should not be higher than 18 V. When patients ejaculated, the stimulation should stop immediately, or retrograde ejaculation occurs (4,30).
It may be of interest to note that we also collected retrograde semen species in the present study. No retrograde fractions were found in the EEJ treatment, whereas retrograde fractions were found in other PAE or SCI patients which are not enrolled in this study.
Few limitations in our study should be noted. The main limitation is that only a small number of patients were included in the present study because the study was undertaken in a single institution and the morbidity of PAE is rather low. The second limitation of the present study is that there is not a definition of PVS-refractory. There are totally twenty papers about the diagnosis and treatment for PAE from 1988 until now. And according to the few literatures, no exact definition of PVS-refractory was mentioned. In our study, these PAE patients were at least performed twice unsuccessful PVS procedures which need our further studies. The third limitation of the present study is the absence of pregnancy and reproductive outcomes of surgical methods like MESA, PESA and TESA for PAE-refractory patients which means a lack of comprehensive comparative study with EEJ.
Finally, in our study, all patients ejaculated successfully following their failure with PVS, the cycle fecundity of IUI and ICSI were 38.5% and 18.8% respectively, which offers an encouraging pregnancy opportunity for men with PAE. We conclude that EEJ combined with assisted reproductive technology may be an alternative choice of treatment in PVS-refractory patients with PAE.
Acknowledgements
None.
Footnote
Conflicts of Interest: The authors have no conflicts of interest to declare.
Ethical Statement: The study protocol was approved by the Departmental Ethics Committee of Tongji Medical College, Huazhong University of Science and Technology (No. TJ-C20160112).
References
- Ralph DJ, Wylie KR. Ejaculatory disorders and sexual function. BJU Int 2005;95:1181-6. [Crossref] [PubMed]
- Heruti RJ, Katz H, Menashe Y, et al. Treatment of male infertility due to spinal cord injury using rectal probe electroejaculation: the Israeli experience. Spinal Cord 2001;39:168-75. [Crossref] [PubMed]
- Sønksen J, Biering-Sørensen F, Kristensen JK. Ejaculation induced by penile vibratory stimulation in men with spinal cord injuries. The importance of the vibratory amplitude. Paraplegia 1994;32:651-60. [PubMed]
- Brackett NL, Ead DN, Aballa TC, et al. Semen retrieval in men with spinal cord injury is improved by interrupting current delivery during electroejaculation. J Urol 2002;167:201-3. [Crossref] [PubMed]
- Brackett NL, Ibrahim E, Iremashvili V, et al. Treatment for ejaculatory dysfunction in men with spinal cord injury: an 18-year single center experience. J Urol 2010;183:2304-8. [Crossref] [PubMed]
- Hsiao W, Deveci S, Mulhall JP. Outcomes of the management of post-chemotherapy retroperitoneal lymph node dissection-associated anejaculation. BJU Int 2012;110:1196-200. [Crossref] [PubMed]
- Gerig NE, Meacham RB, Ohl DA. Use of electroejaculation in the treatment of ejaculatory failure secondary to diabetes mellitus. Urology 1997;49:239-42. [Crossref] [PubMed]
- Fode M, Krogh-Jespersen S, Brackett NL, et al. Male sexual dysfunction and infertility associated with neurological disorders. Asian J Androl 2012;14:61-8. [Crossref] [PubMed]
- Schmiegelow ML, Sommer P, Carlsen E, et al. Penile vibratory stimulation and electroejaculation before anticancer therapy in two pubertal boys. J Pediatr Hematol Oncol 1998;20:429-30. [Crossref] [PubMed]
- Soeterik TF, Veenboer PW, Lock TM. Electroejaculation in psychogenic anejaculation. Fertil Steril 2014;101:1604-8. [Crossref] [PubMed]
- Meacham R. Management of psychogenic anejaculation. J Androl 2003;24:170-1. [Crossref] [PubMed]
- Hovav Y, Kafka I, Horenstein E, et al. Prostatic massage as a method for obtaining spermatozoa in men with psychogenic anejaculation. Fertil Steril 2000;74:184-5. [Crossref] [PubMed]
- Fahmy I, Kamal A, Metwali M, et al. Vigorous prostatic massage: a simple method to retrieve spermatozoa for intracytoplasmic sperm injection in psychogenic anejaculation: case report. Hum Reprod 1999;14:2050-3. [Crossref] [PubMed]
- Hovav Y, Dan-Goor M, Yaffe H, et al. Nocturnal sperm emission in men with psychogenic anejaculation. Fertil Steril 1999;72:364-5. [Crossref] [PubMed]
- Meng X, Fan L, Liu J, et al. Fresh semen quality in ejaculates produced by nocturnal emission in men with idiopathic anejaculation. Fertil Steril 2013;100:1248-52. [Crossref] [PubMed]
- Silber SJ, Nagy ZP, Liu J, et al. Conventional IVF versus ICSI (intracytoplasmic sperm injection) for patients requiring microsurgical sperm aspiration (MESA). Hum Reprod 1994;9:1705-9. [Crossref] [PubMed]
- Lin YH, Hwang JL, Tsai YL. Percutaneous epididymal sperm aspiration in psychogenic anejaculation during IVF. A report of two cases. J Reprod Med 1999;44:894-6. [PubMed]
- Alrabeeah K, Yafi F, Flageole C, et al. Testicular sperm aspiration for nonazoospermic men: sperm retrieval and ICSI outcomes. Urology 2014;84:1342-6. [Crossref] [PubMed]
- Almagor M, Dan-Goor M, Hovav Y, et al. Antisperm antibodies in men with psychogenic anejaculation. Arch Androl 1998;41:1-4. [Crossref] [PubMed]
- Stewart DE, Ohl DA. Idiopathic anejaculation treated by electroejaculation. Int J Psychiatry Med 1989;19:263-8. [Crossref] [PubMed]
- Vanderschueren D, Spiessens C, Kiekens C, et al. Successful treatment of idiopathic anejaculation with electroejaculation after microsurgical vas aspiration. Hum Reprod 1998;13:370-1. [Crossref] [PubMed]
- Kiekens C, Spiessens C, Duyck F, et al. Pregnancy after electroejaculation in combination with intracytoplasmic sperm injection in a patient with idiopathic anejaculation. Fertil Steril 1996;66:834-6. [Crossref] [PubMed]
- Gat I, Maman E, Yerushalmi G, et al. Electroejaculation combined with intracytoplasmic sperm injection in patients with psychogenic anejaculation yields comparable results to patients with spinal cord injuries. Fertil Steril 2012;97:1056-60. [Crossref] [PubMed]
- Hovav Y, Yaffe H, Zentner B, et al. The use of ICSI with fresh and cryopreserved electroejaculates from psychogenic anejaculatory men. Hum Reprod 2002;17:390-2. [Crossref] [PubMed]
- Shull GR, Sprenkle DH. Retarded ejaculation reconceptualization and implications for treatment. J Sex Marital Ther 1980;6:234-46. [Crossref] [PubMed]
- Rowan RL, Howley TF. Ejaculatory sterility. Fertil Steril 1965;16:768-70. [Crossref] [PubMed]
- Hovav Y, Shotland Y, Yaffe H, et al. Electroejaculation and assisted fertility in men with psychogenic anejaculation. Fertil Steril 1996;66:620-3. [Crossref] [PubMed]
- Frankel HL, Mathias CJ. Severe hypertension in patients with high spinal cord lesions undergoing electro-ejaculation--management with prostaglandin E2. Paraplegia 1980;18:293-9. [PubMed]
- Brackett NL, Lynne CM. The method of assisted ejaculation affects the outcome of semen quality studies in men with spinal cord injury. NeuroRehabilitation 2000;15:89-100. [PubMed]
- Sønksen J, Ohl DA, Wedemeyer G. Sphincteric events during penile vibratory ejaculation and electroejaculation in men with spinal cord injuries. J Urol 2001;165:426-9. [Crossref] [PubMed]


